
හැදින්වීම
Understanding the dynamics of genetic disorders is crucial for effective patient care, particularly regarding phenylketonuria (PKU). This rare metabolic condition has significant implications for affected families. Genetic counselors play a pivotal role in navigating the complexities of PKU inheritance patterns. They offer insights that empower families to make informed reproductive choices.
Despite advancements in screening and treatment, many families still face challenges in managing this condition. Key insights into PKU inheritance can enhance understanding and improve counseling strategies for those impacted. By focusing on these insights, we can better support families in their journey.
Define Phenylketonuria and Its Inheritance Pattern
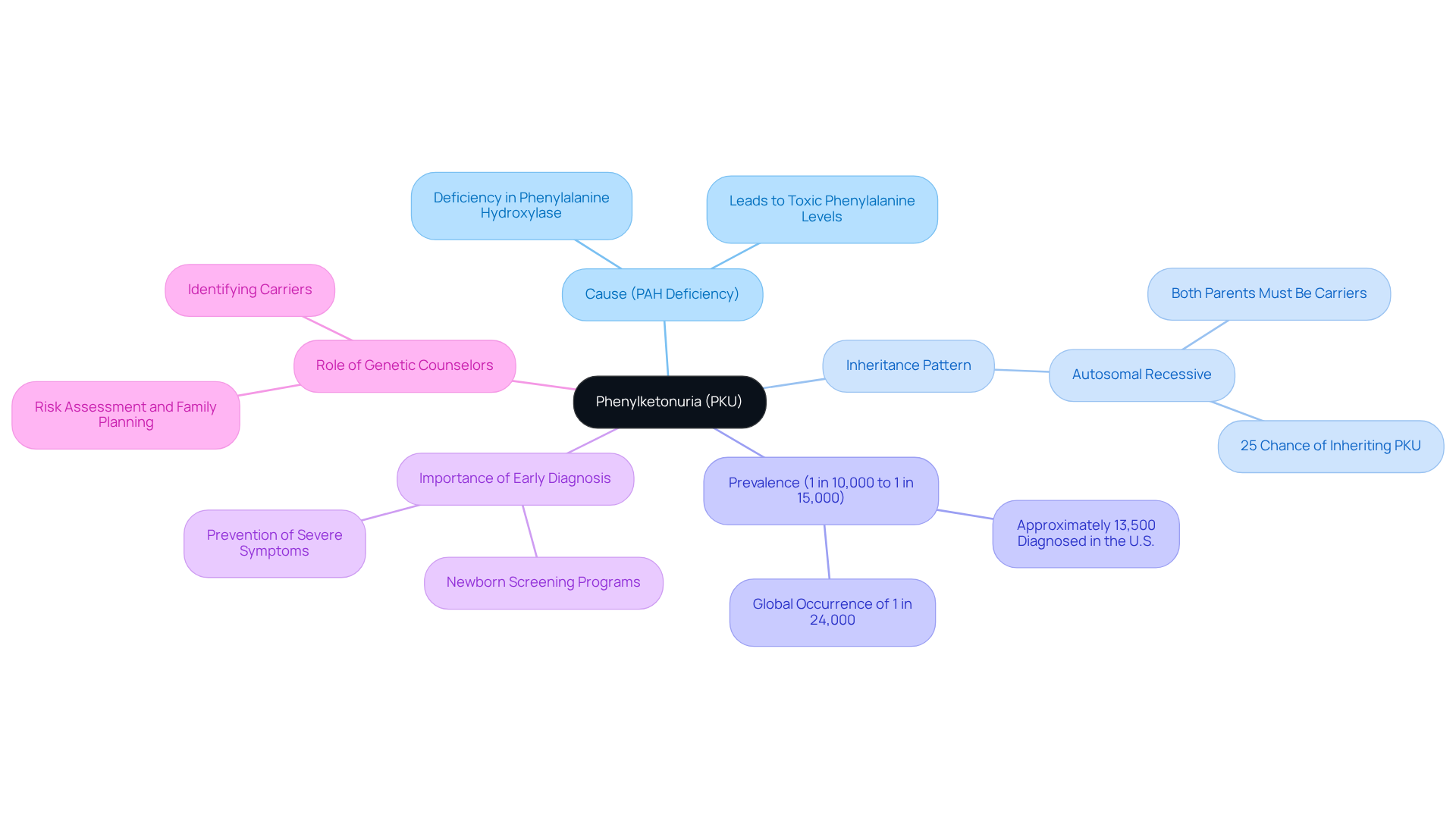
Phenylketonuria (PKU) is a rare inherited metabolic disorder caused by a deficiency in the enzyme phenylalanine hydroxylase (PAH), essential for metabolizing the amino acid phenylalanine. This condition follows a PKU inheritance pattern, meaning an individual must inherit two copies of the mutated PAH gene-one from each parent-to exhibit the disorder. If both parents are carriers of the mutation, there is a 25% chance with each pregnancy that their child will inherit PKU.
Recent studies indicate that PKU affects approximately 1 in 10,000 to 1 in 15,000 infants in the United States. This statistic underscores the importance of early diagnosis through newborn screening programs. Genetic counselors are crucial in elucidating the PKU inheritance pattern, which aids in risk assessments and family planning discussions for those impacted by PKU.
Furthermore, case studies highlight that awareness of autosomal recessive inheritance is vital for identifying carriers and effectively managing the condition through genetic counseling. This understanding empowers families to make informed decisions regarding their reproductive options and the health of future generations.
Explore the History of PKU Diagnosis
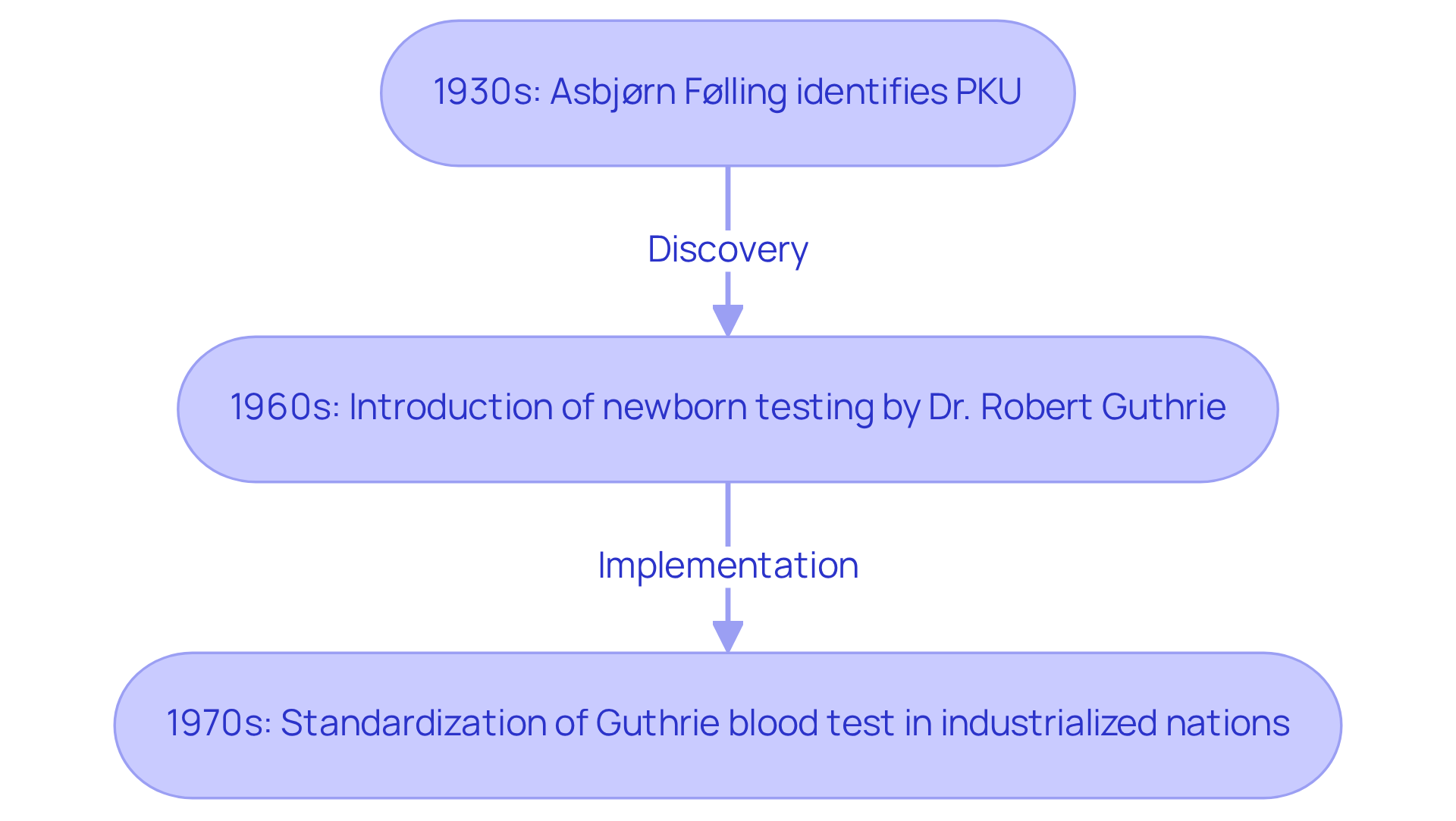
The diagnosis of phenylketonuria (PKU) is rooted in the 1930s, when Norwegian physician Asbjørn Følling first identified the disorder in siblings with intellectual disabilities. This discovery was pivotal, laying the groundwork for understanding the genetic basis of PKU.
A significant advancement occurred in the 1960s with the introduction of newborn testing, spearheaded by Dr. Robert Guthrie. This monumental leap in public health enabled early detection of PKU, allowing for immediate dietary interventions that could prevent severe neurological damage. The Guthrie blood test became a cornerstone of newborn evaluation, facilitating routine testing that has since become standard practice in nearly every industrialized nation by the mid-1970s.
Understanding this historical context is crucial for genetic advisors, as it underscores the evolution of treatment strategies and the essential role of early diagnosis in enhancing patient outcomes. PKU affects approximately 1 in 15,000 individuals, which highlights the importance of comprehensive newborn evaluation programs in safeguarding health.
Case studies further illustrate that timely intervention can lead to normal developmental trajectories for affected children, reinforcing the critical role of these programs in public health discussions.
Analyze Clinical Presentation and Epidemiology of PKU
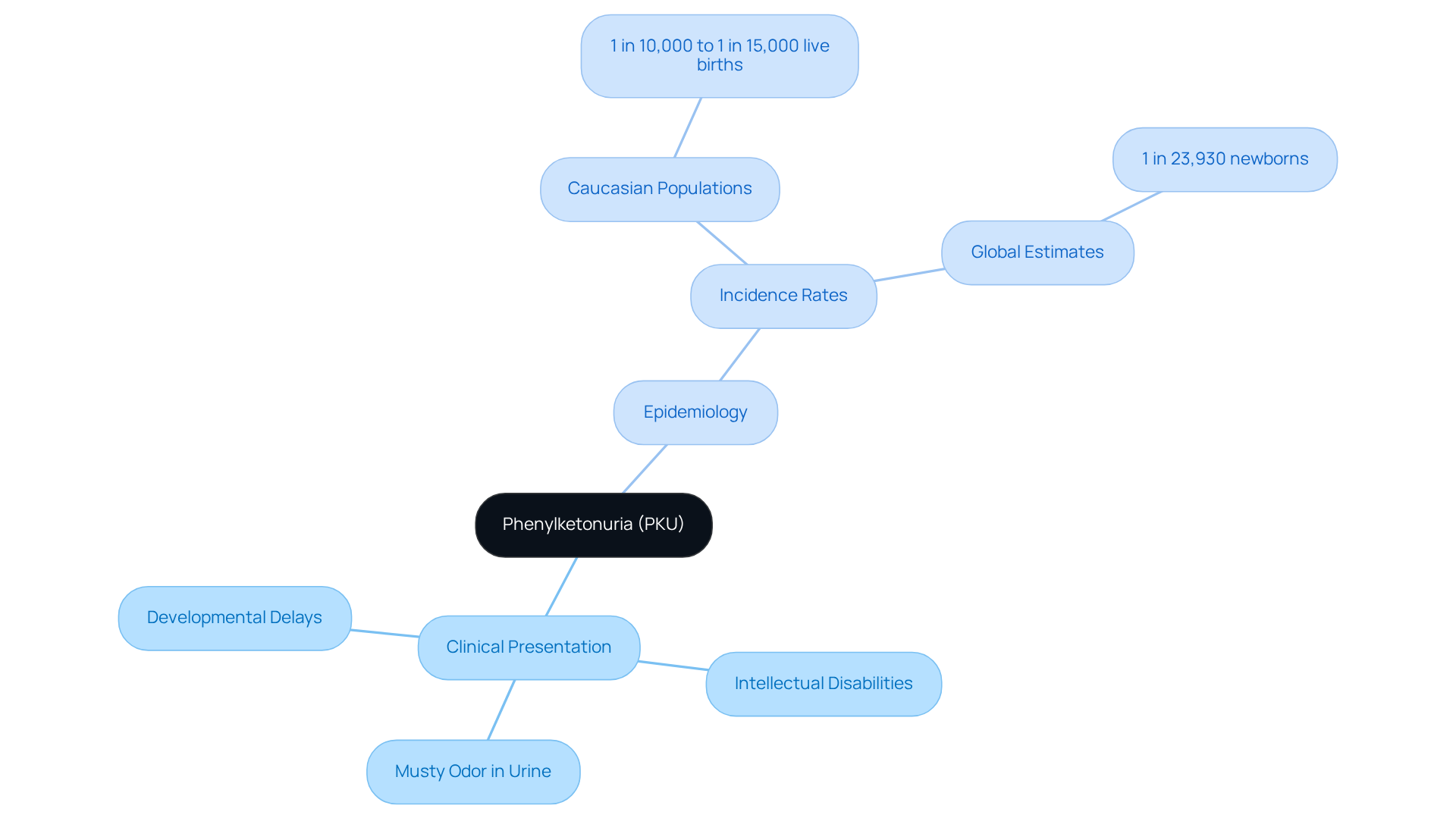
Phenylketonuria (PKU) typically manifests in infancy, characterized by developmental delays, intellectual disabilities, and a distinctive musty odor in urine. If left untreated, PKU can result in severe cognitive impairment.
The incidence of PKU varies globally, with higher rates observed in Caucasian populations, estimated at approximately 1 in 10,000 to 1 in 15,000 live births. Understanding the clinical presentation and epidemiology of PKU is crucial for genetic counselors. This knowledge enables them to identify at-risk individuals and provide appropriate guidance to families regarding assessment and management.
Detail the Diagnosis and Screening Methods for PKU
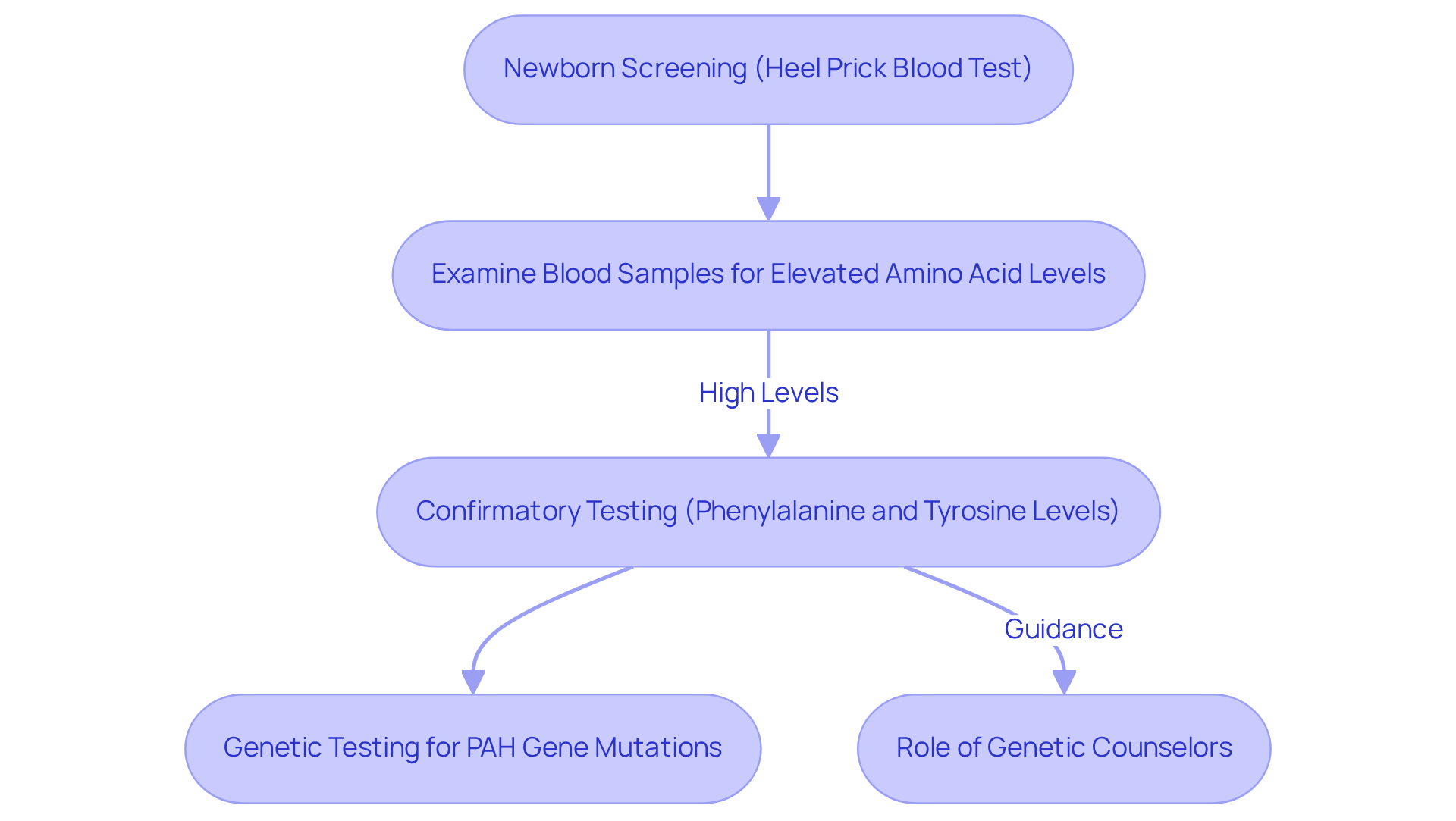
Phenylketonuria (PKU) is primarily diagnosed through newborn screening, which is typically performed within the first few days of life via a heel prick blood test. This method allows for the examination of blood samples for elevated amino acid levels. If these levels are found to be high, confirmatory testing is required. This follow-up assessment measures both phenylalanine and tyrosine levels and may include genetic testing to identify mutations in the PAH gene.
The significance of early diagnosis is paramount; it facilitates immediate dietary interventions that are crucial for preventing neurological damage. Recent updates in 2026 have highlighted advancements in testing techniques, ensuring greater accuracy and reliability in detecting PKU.
Genetic counselors play a vital role in this process, guiding families through the evaluation journey and underscoring the critical nature of timely diagnosis and confirmatory testing. Case studies further illustrate the effectiveness of these methods, demonstrating how early detection has led to improved outcomes for affected individuals. For example, timely screening has been shown to increase the likelihood of early dietary management, significantly reducing the risk of complications associated with delayed treatment.
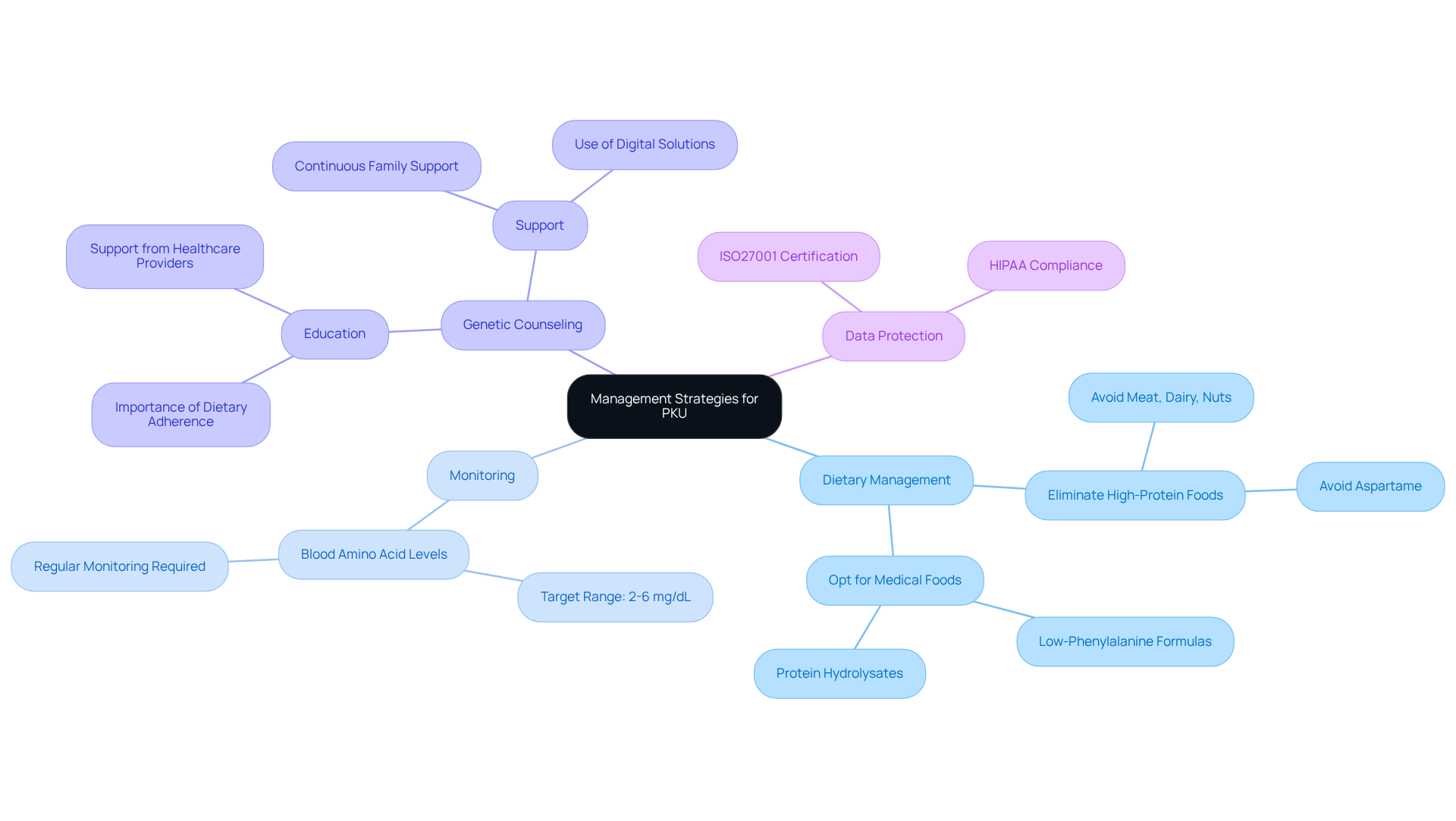
Outline Management Strategies for PKU
Effective management of phenylketonuria (PKU) necessitates a strict dietary plan that limits the intake of specific amino acids. Patients must eliminate high-protein foods, such as meat, dairy, and nuts, from their diets. Instead, they should opt for specially formulated medical foods that are low in certain amino acids.
Regular monitoring of blood amino acid levels is essential, with recommended targets for children set between 2 mg/dL and 6 mg/dL (120 to 360 micromol/L). This ongoing assessment is crucial to ensure that levels remain within a safe range, thereby preventing potential cognitive and developmental issues associated with elevated phenylalanine.
Genetic advisors play a vital role in educating families about the importance of dietary adherence and the necessity for continuous support from specialized healthcare providers. TrakGene’s innovative digital solutions, including pedigree chart creation, assist genetic professionals in visualizing family histories and understanding the PKU inheritance pattern. Additionally, genomic health records enhance data management and patient support.
Furthermore, TrakGene’s commitment to data protection, ensuring HIPAA and GDPR compliance through ISO27001 certification, provides genetic counselors with the assurance that patient information is handled securely.
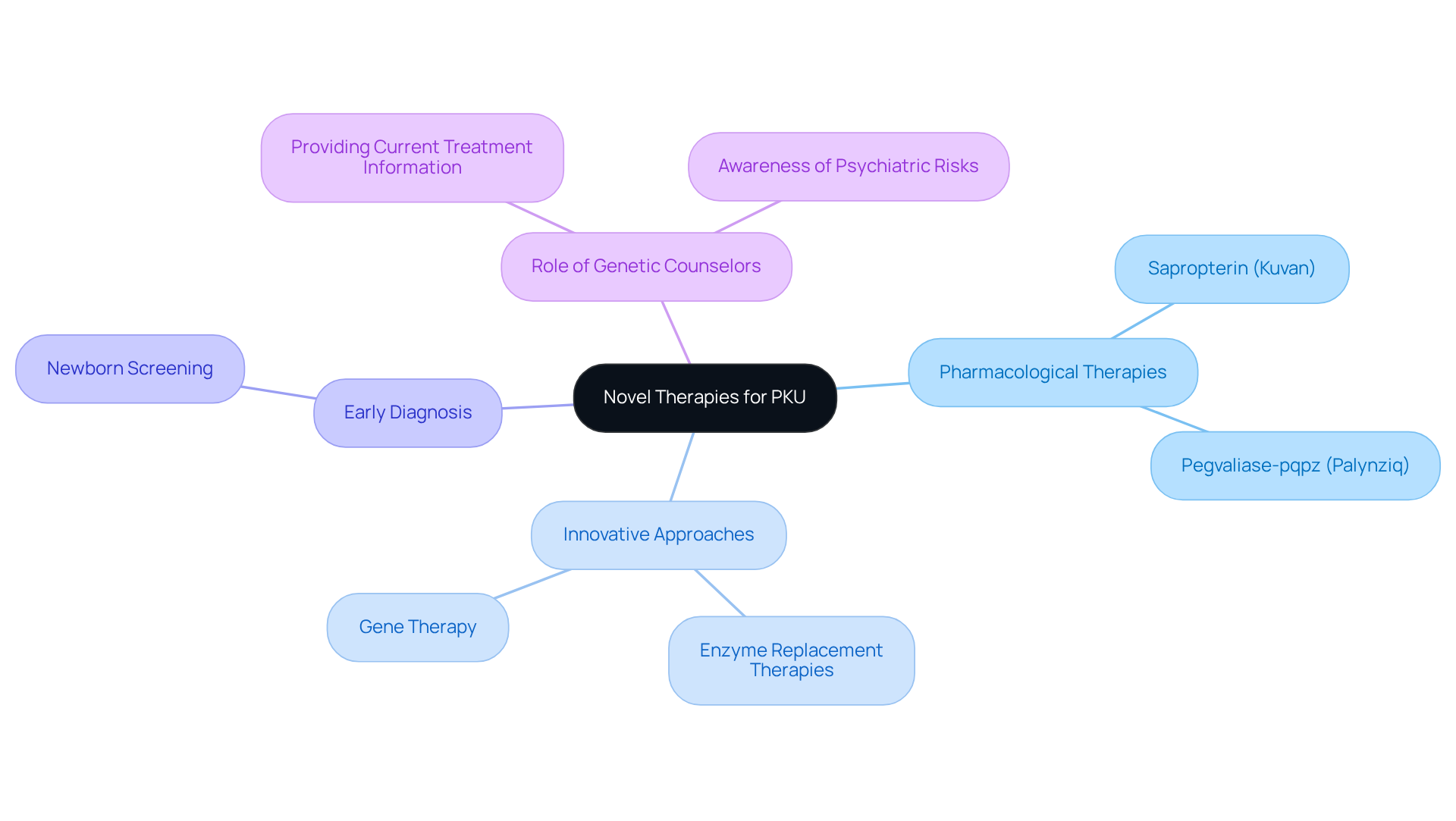
Introduce Novel Therapies for PKU
Recent advancements in the treatment of phenylketonuria (PKU) have introduced significant pharmacological therapies. Notably, sapropterin (Kuvan) enhances the ability of some patients to metabolize phenylalanine effectively. Furthermore, pegvaliase-pqpz (Palynziq) has been approved for adults when current therapy is insufficient, marking a substantial improvement in treatment options.
Innovative approaches, including enzyme replacement therapies and gene therapy, are being explored as promising alternatives to traditional dietary restrictions. These novel therapies aim to alleviate the burden of strict dietary compliance and enhance the overall quality of life for individuals living with PKU.
Early diagnosis through newborn screening is critical, as it identifies nearly all cases of PKU and is mandated in all 50 states in the U.S. This early intervention is essential in preventing major developmental complications.
Genetic counselors should remain informed about these developments to provide families with the most current information regarding treatment options. This includes awareness of the psychiatric risks associated with adolescent cannabis use.
නිගමනය
In conclusion, phenylketonuria (PKU) is a complex genetic disorder that highlights the necessity of understanding its inheritance patterns, diagnosis, and management strategies. Genetic counselors play a critical role in guiding families through the nuances of PKU, from identifying carriers to discussing reproductive options. By comprehending the intricacies of PKU’s autosomal recessive inheritance, families can make informed decisions that significantly impact future generations.
Advancements in newborn screening have transformed the early detection and intervention of PKU, allowing for improved management of the condition. The clinical presentation and epidemiology of PKU underscore the importance of awareness among healthcare professionals, enabling them to recognize symptoms and provide timely support. Additionally, the exploration of management strategies, including dietary restrictions and emerging therapies, illustrates the evolving landscape of PKU treatment, emphasizing the need for continuous education and adaptation in care approaches.
As the field of genetic counseling advances, it is increasingly vital to stay informed about the latest research and treatment options for PKU. Families facing PKU must be equipped with knowledge and resources to navigate this journey, ensuring that affected individuals can lead fulfilling lives. The significance of early diagnosis and comprehensive management cannot be overstated, as they are crucial in mitigating the challenges posed by this disorder.
නිතර අසනු ලබන ප්රශ්න
What is phenylketonuria (PKU)?
Phenylketonuria (PKU) is a rare inherited metabolic disorder caused by a deficiency in the enzyme phenylalanine hydroxylase (PAH), which is essential for metabolizing the amino acid phenylalanine.
How is PKU inherited?
PKU follows an autosomal recessive inheritance pattern, meaning an individual must inherit two copies of the mutated PAH gene-one from each parent-to exhibit the disorder. If both parents are carriers of the mutation, there is a 25% chance with each pregnancy that their child will inherit PKU.
How common is PKU in the United States?
PKU affects approximately 1 in 10,000 to 1 in 15,000 infants in the United States.
Why is early diagnosis of PKU important?
Early diagnosis through newborn screening programs is crucial because it allows for immediate dietary interventions that can prevent severe neurological damage.
Who plays a key role in understanding the inheritance pattern of PKU?
Genetic counselors are essential in elucidating the PKU inheritance pattern, aiding in risk assessments and family planning discussions for those impacted by PKU.
What historical advancements contributed to the diagnosis of PKU?
The diagnosis of PKU began in the 1930s with Asbjørn Følling’s identification of the disorder. A significant advancement occurred in the 1960s with the introduction of newborn testing by Dr. Robert Guthrie, which enabled early detection and intervention.
What is the Guthrie blood test?
The Guthrie blood test is a screening method that became a cornerstone of newborn evaluation, facilitating routine testing for PKU that has become standard practice in nearly every industrialized nation since the mid-1970s.
What impact does timely intervention have on children with PKU?
Timely intervention can lead to normal developmental trajectories for affected children, highlighting the critical role of early diagnosis and treatment in improving patient outcomes.






