
pengenalan
Genomic testing is pivotal in modern healthcare, offering critical insights embedded within an individual’s DNA that can significantly influence health decisions and treatment strategies. This article examines the vital role of genomic testing in genetic counseling, highlighting how it enables counselors to navigate complex genetic landscapes, ultimately improving health outcomes.
However, as the field progresses, notable challenges persist – how can counselors effectively interpret results and convey their implications to families? This exploration aims to reveal the transformative potential of genomic testing while addressing the urgent questions that emerge in its application.
Define Genomic Testing and Its Importance in Genetic Counseling
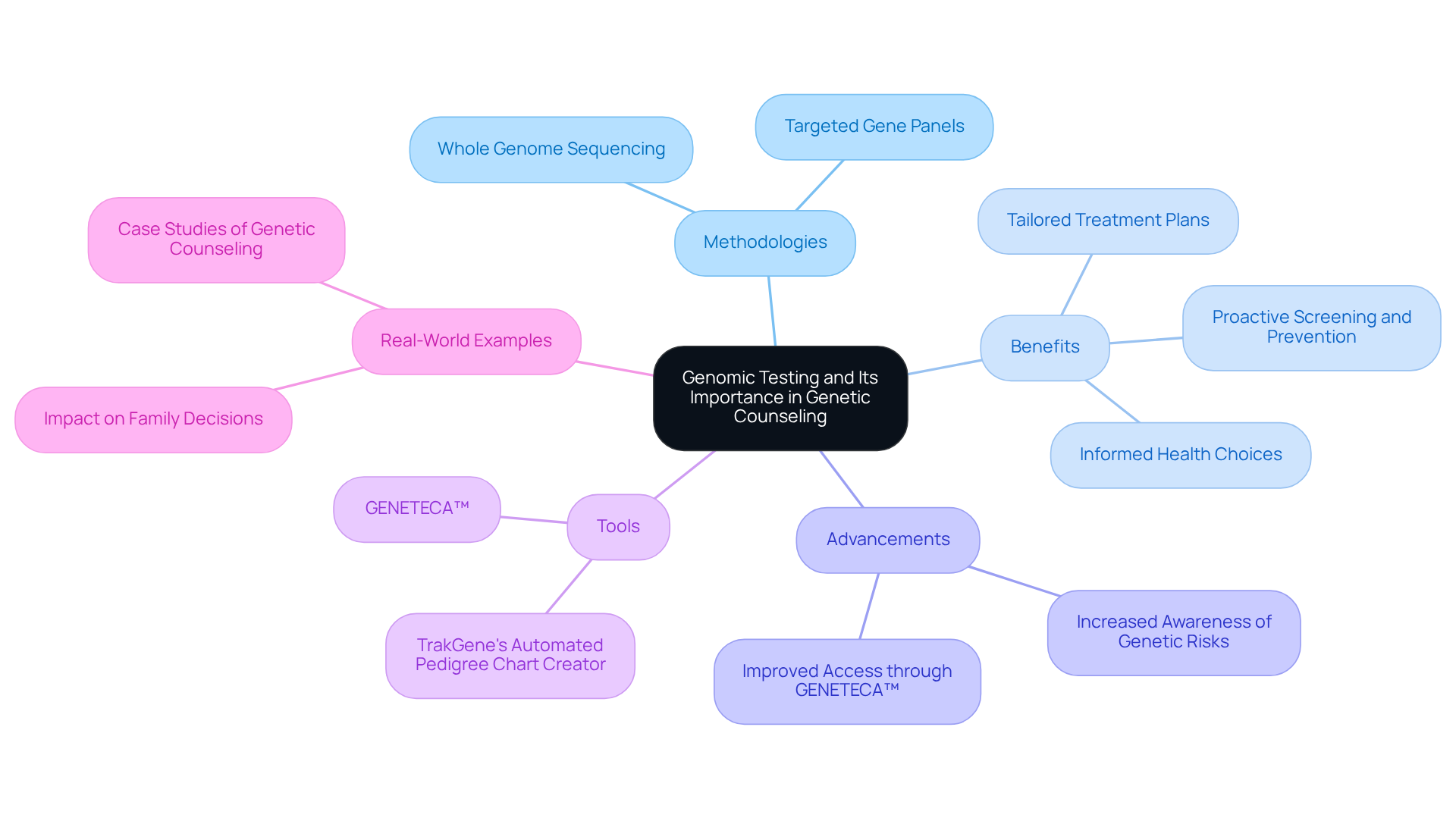
Genomic testing UK is a critical process that examines an individual’s DNA to uncover variations influencing health, disease susceptibility, and treatment responses. This analysis employs methodologies such as whole genome sequencing and targeted gene panels, offering insights into inherited conditions, disease predispositions, and medication responses.
A comprehensive understanding of DNA testing is essential in hereditary guidance. It equips counselors to assist individuals in navigating complex genetic information, empowering them to make informed health choices for themselves and their families. By analyzing genetic data, counselors can identify at-risk individuals, recommend preventive measures, and tailor treatment plans. This proactive approach not only enhances patient outcomes but also fosters a culture of informed health management.
Recent advancements in genetic analysis have significantly influenced health choices. For instance, studies reveal that nearly 90% of participants were unaware of their DNA risk prior to disclosure, highlighting the importance of hereditary assessments in raising awareness and facilitating early interventions. Additionally, tools like GENETECA™ have simplified access to DNA assessments, increasing the proportion of cancer patients receiving recommended germline evaluations from 22% to 94% within 18 months of its release. This shift underscores the growing recognition of genomic testing in the UK and its role in personalized medicine, where targeted therapies can improve outcomes for conditions with hereditary components, such as ovarian and uterine cancers.
TrakGene’s automated pedigree chart creator enhances this landscape by providing intuitive tools for capturing family history and analyzing hereditary information. This solution simplifies the process for counselors while ensuring secure access to integrated health records and cancer risk evaluation tools, thereby improving engagement and data security. The partnership with New South Wales Health further strengthens this offering, ensuring counselors have access to extensive resources and support.
Real-world examples illustrate the substantial impact of genomic analysis on individual decision-making. For example, hereditary analysis results can inform family members about their cancer risks, promoting proactive screening and prevention strategies. Furthermore, individuals who receive timely hereditary guidance and assessments are better equipped to manage their health journeys, leading to improved care coordination and outcomes. As the field of DNA analysis continues to evolve, the role of genetic advisors remains vital in ensuring that patients benefit from these advancements. Addressing barriers to equitable access and the financial challenges associated with care plans is crucial for enhancing the overall effectiveness of genomic evaluations across diverse populations.
Explore the Methodology of Genomic Testing: Techniques and Processes
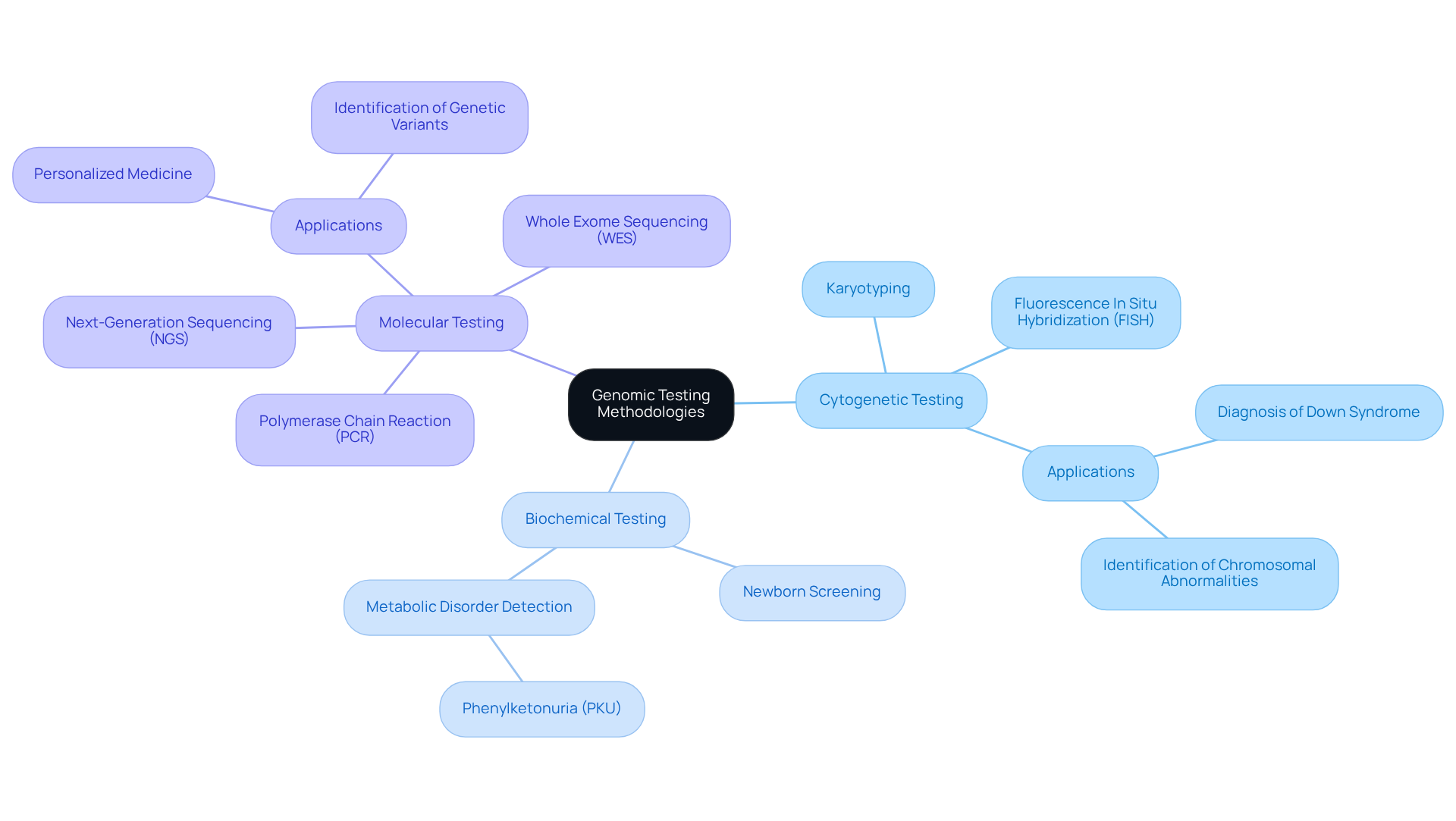
Genomic testing UK methodologies can be categorized into three primary types: cytogenetic testing, biochemical testing, and molecular testing.
-
Cytogenetic Testing: This method analyzes chromosomes for structural irregularities, such as deletions or duplications, which can lead to hereditary disorders. Common techniques include karyotyping and fluorescence in situ hybridization (FISH). These techniques are essential for diagnosing conditions like Down syndrome and other chromosomal abnormalities.
-
Biochemical Testing: This method assesses the presence of specific proteins or metabolites in the body, serving as indicators of hereditary conditions. For instance, newborn screening tests for metabolic disorders often rely on biochemical analysis to detect conditions like phenylketonuria (PKU) early in life, allowing for timely intervention.
-
Molecular testing: As the most advanced form of genomic testing UK, this focuses on the DNA sequence itself. Techniques such as polymerase chain reaction (PCR), next-generation sequencing (NGS), and whole exome sequencing (WES) facilitate the identification of variants at a granular level. These technologies are crucial in personalized medicine, enabling customized treatment strategies based on an individual’s biological composition.
By comprehending these approaches, counselors can effectively convey the evaluation procedure to individuals, clarifying the implications of various assessments and their significance to personal health outcomes. This knowledge is essential as the field of genetic analysis continues to evolve, with advancements in technology enhancing diagnostic capabilities and healthcare.
Interpret Genomic Testing Results: Implications for Patients and Families
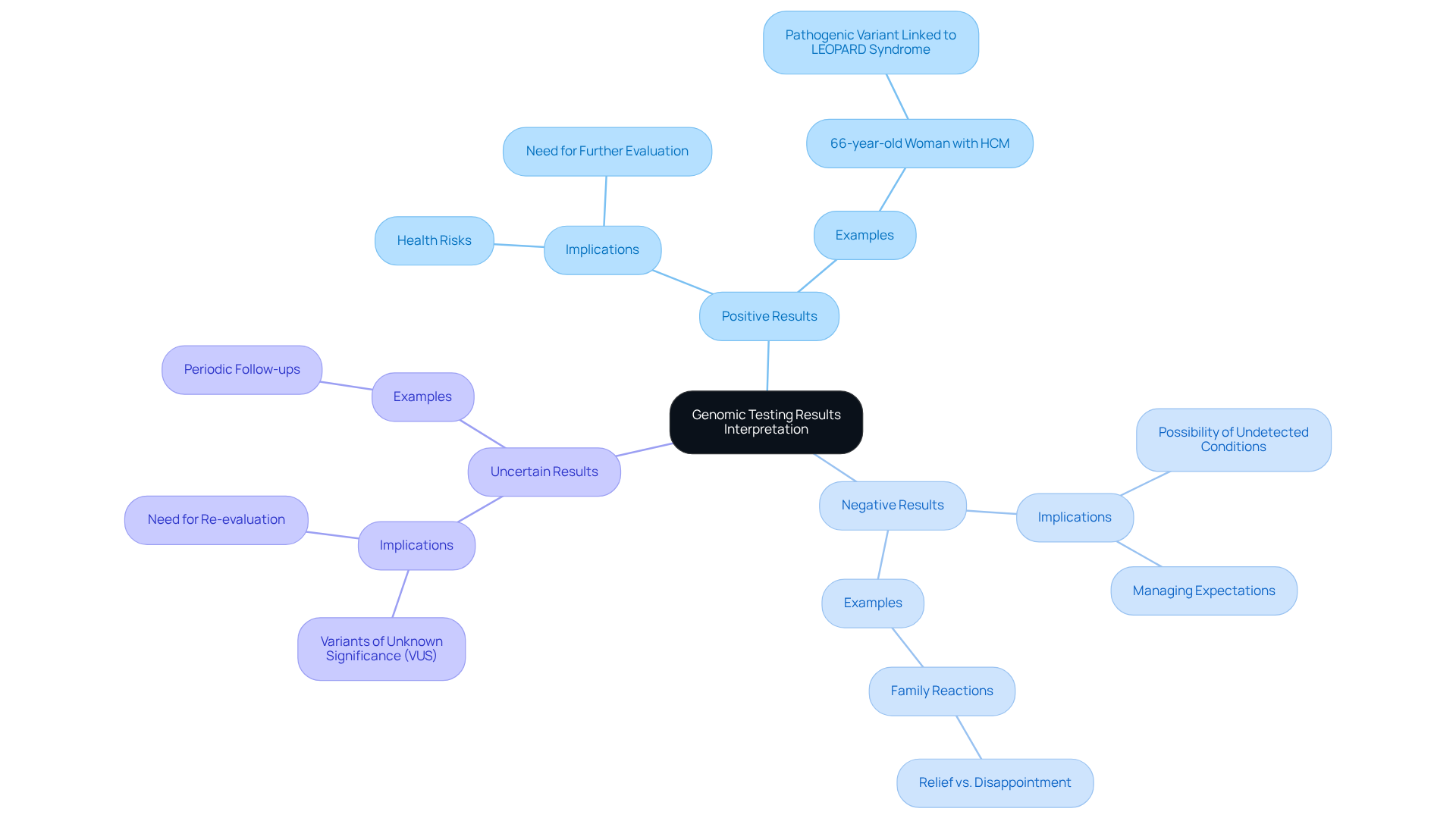
Interpreting genomic testing results necessitates a nuanced understanding of the clinical significance of identified variants, which can be categorized as positive, negative, or uncertain. Each classification carries distinct implications for patients and their families.
-
Positive Results: These results indicate the presence of a hereditary variant linked to a specific condition. Counselors must clearly communicate the implications, including potential health risks and the need for further evaluation or ongoing monitoring. For instance, a harmful variant found in an individual may prompt relatives to consider hereditary testing, as seen in cases where familial links to disorders such as hypertrophic cardiomyopathy (HCM) were confirmed through genomic analysis. A notable example involves a 66-year-old woman diagnosed with HCM who was found to have a pathogenic variant associated with LEOPARD syndrome, despite lacking classic symptoms. This case illustrates the challenges of identifying pathogenic variants in individuals with nonclassic presentations.
-
Negative Results: While negative results suggest that no pathogenic variants were detected, it is essential to discuss their limitations. Negative findings do not eliminate the possibility of undetected hereditary conditions, as evidenced by instances where individuals with significant family histories received negative results yet still faced health issues. This underscores the necessity for genetic counselors to manage expectations and provide reassurance regarding the ongoing nature of genetic risk assessment. For example, family reactions to negative results can vary significantly, highlighting the importance of tailored counseling strategies.
-
Uncertain Results: Results classified as uncertain often involve variants of unknown significance (VUS), which can pose particular challenges for families. Counselors should offer support and guidance on next steps, including the potential for re-evaluation as new information becomes available. For example, an individual who receives a VUS may benefit from periodic follow-ups to reassess the variant’s significance as research progresses.
Effective communication of these results is crucial for fostering patient understanding and emotional support. By equipping families with the knowledge to navigate their health choices, counselors play a vital role in managing the complexities of DNA analysis results.
Integrate Genomic Testing into Clinical Practice: Best Practices for Counselors
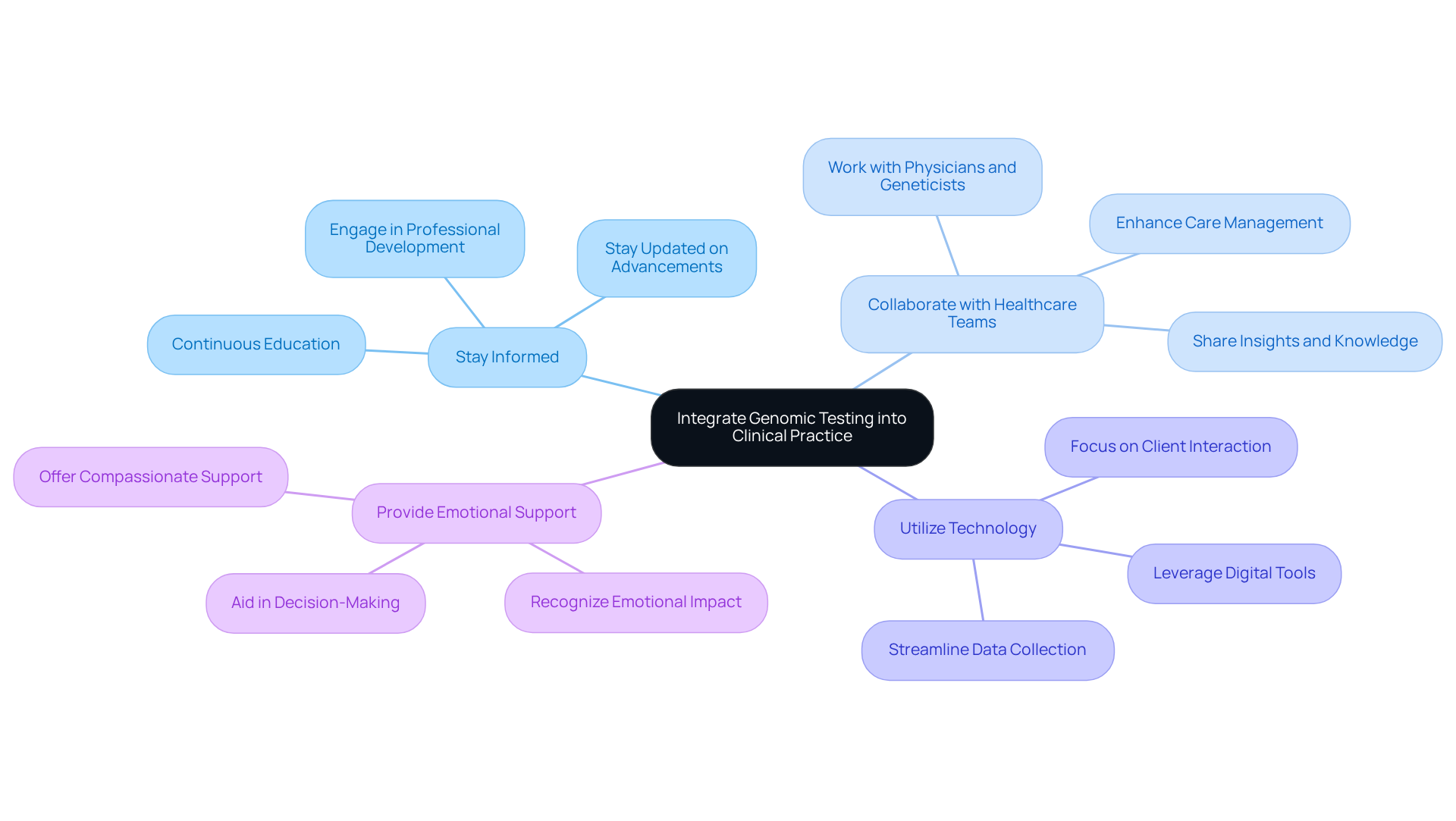
To effectively integrate genomic testing into clinical practice, genetic counselors should adopt the following best practices:
-
Stay Informed: Continuous education on the latest advancements in genomic testing and technologies is essential. Engaging in professional development opportunities allows counselors to remain current with evolving practices, which is crucial given the rapid advancements in the field. Recent statistics indicate that enrollment in counseling programs focused on heredity has surged by 53% from 2018 to 2023, reflecting the increasing demand for skilled professionals in this area.
-
Collaborate with Healthcare Teams: Close cooperation with physicians, geneticists, and other healthcare professionals is vital for a comprehensive approach to care. This collaboration not only promotes the exchange of insights but also enhances the overall management of hereditary conditions. Research has demonstrated that incorporating hereditary advisors into diverse care groups significantly improves outcomes and satisfaction for individuals, as they provide specialized knowledge in risk evaluation and treatment strategy.
-
Utilize Technology: Leveraging digital tools and platforms, such as TrakGene’s intuitive pedigree chart maker, can streamline data collection and analysis. This tool simplifies family history gathering and enhances health record management with integrated risk evaluation, enabling counselors to focus more on client interaction rather than administrative duties. The incorporation of technology into practice has been shown to reduce the time counselors spend on paperwork, allowing them to dedicate more attention to direct client care.
-
Provide Emotional Support: Recognizing the emotional impact of genomic testing results on patients and families is crucial. Counselors should offer compassionate support and resources to help them navigate their feelings and decisions. The ethos of hereditary counseling emphasizes empathy and patient-centered care, which are essential in assisting families to cope with the complexities of hereditary information. As Jehannine Austin states, “Counseling regarding heredity is a psychotherapeutic process of assisting individuals in understanding hereditary information, and aiding them in utilizing that information in accordance with their values, needs, and desires.”
By implementing these best practices, genetic counselors can enhance the integration of genomic testing UK into their clinical workflows, ultimately improving patient outcomes and satisfaction.
Kesimpulan
Genomic testing stands as a pivotal advancement in healthcare, particularly in the field of genetic counseling. By analyzing an individual’s DNA, this process yields critical insights into health risks, disease predispositions, and treatment responses. Such information empowers patients to take control of their health decisions. The incorporation of genomic testing into clinical practice not only improves patient outcomes but also cultivates an environment of informed health management, which is essential for navigating the complexities of genetic information.
The article outlines several key components of genomic testing, including its methodologies, result interpretation, and recommended practices for genetic counselors. Techniques such as cytogenetic, biochemical, and molecular testing each play a crucial role in identifying hereditary conditions. Additionally, comprehending the implications of positive, negative, and uncertain results is vital for counselors to effectively support patients and their families. The article further underscores the necessity of ongoing education, collaboration with healthcare teams, and the application of technology to streamline processes and enhance patient care.
As genomic testing continues to advance, its role in personalized medicine is increasingly significant. Genetic counselors are at the forefront of this evolution, equipped with the expertise and tools to guide individuals through their genetic journeys. Embracing these advancements while addressing barriers to equitable access will ensure that all patients can benefit from the power of genomic insights. The imperative is clear: prioritize the integration of genomic testing in clinical practice to revolutionize health management and improve outcomes for diverse populations.
Soalan Lazim
What is genomic testing?
Genomic testing is a process that examines an individual’s DNA to uncover variations that influence health, disease susceptibility, and treatment responses. It utilizes methods such as whole genome sequencing and targeted gene panels.
Why is genomic testing important in genetic counseling?
Genomic testing is important in genetic counseling as it helps counselors provide guidance on complex genetic information, empowering individuals to make informed health choices, identify at-risk individuals, recommend preventive measures, and tailor treatment plans.
How has genomic testing influenced health choices?
Genomic testing has raised awareness about genetic risks, with studies showing that nearly 90% of participants were unaware of their DNA risk before disclosure. This awareness facilitates early interventions and proactive health management.
What advancements have been made in genomic testing tools?
Tools like GENETECA™ have simplified access to DNA assessments, significantly increasing the proportion of cancer patients receiving recommended germline evaluations from 22% to 94% within 18 months of its release.
How does TrakGene enhance the genomic testing process?
TrakGene’s automated pedigree chart creator provides intuitive tools for capturing family history and analyzing hereditary information, improving engagement and data security for counselors while ensuring secure access to health records.
What is the impact of hereditary analysis on individual decision-making?
Hereditary analysis results inform family members about their cancer risks, promoting proactive screening and prevention strategies, and helping individuals manage their health journeys more effectively.
What challenges exist in the field of genomic testing?
Challenges include barriers to equitable access and financial issues associated with care plans, which need to be addressed to enhance the effectiveness of genomic evaluations across diverse populations.




