
introduzione
Understanding blood type inheritance is not merely a genetic curiosity; it is essential in medical practices, familial relationships, and disease susceptibility. This article explores the complexities of blood type inheritance, emphasizing the significance of the ABO gene and its implications for genetic counseling and transfusion compatibility. When the intricacies of blood type inheritance intersect with real-world medical scenarios, the knowledge gained can profoundly influence patient care and health outcomes.
Define Blood Type Inheritance
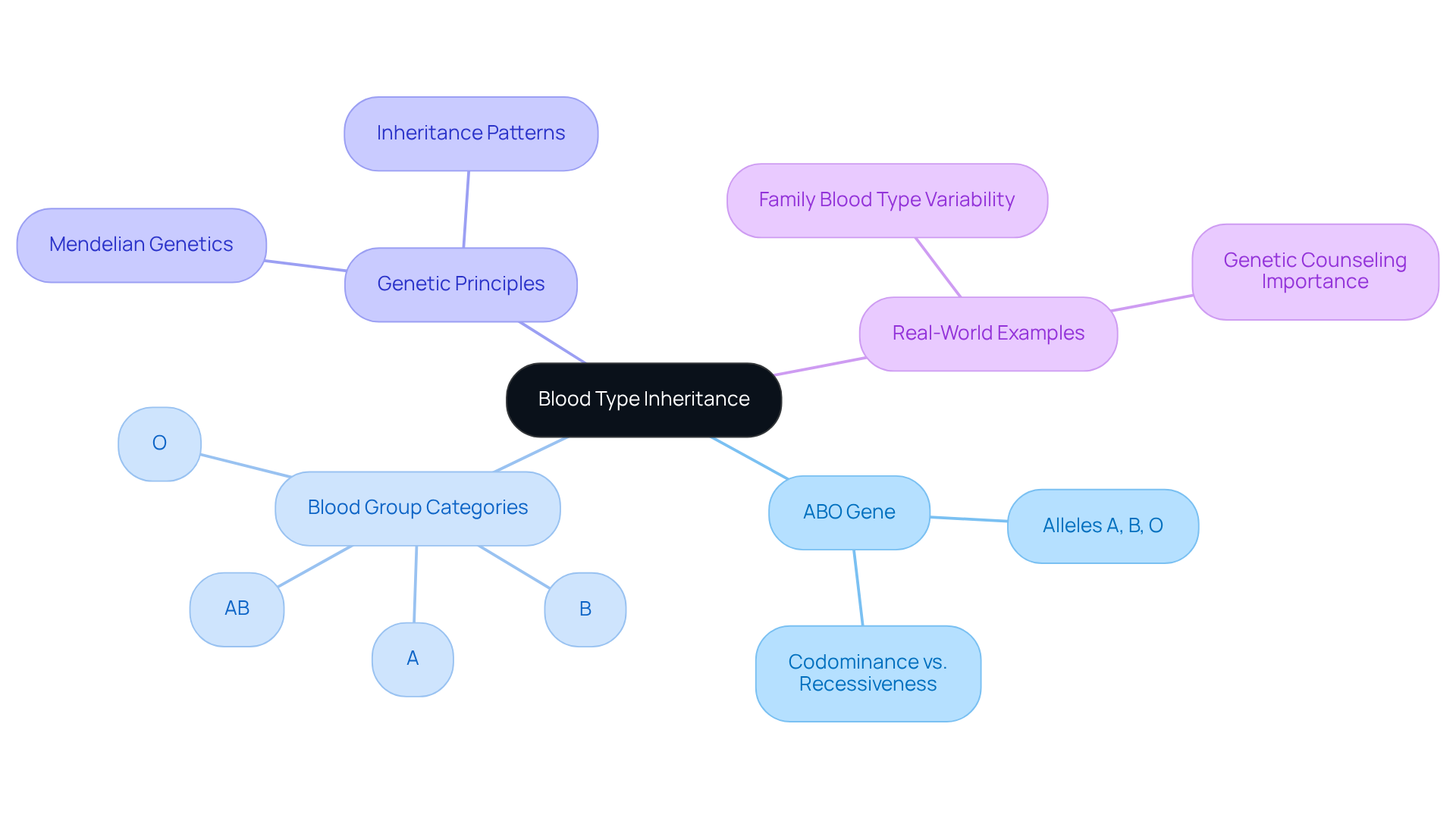
The genetic transfer of traits from parents to their offspring is a fundamental concept in understanding blood type inheritance. Each individual inherits two alleles of the ABO gene-one from each parent-which determines their blood group. The ABO grouping system comprises four primary categories: A, B, AB, and O. These categories are characterized by the presence or absence of specific antigens on the surface of red blood cells. This blood type inheritance pattern adheres to Mendelian genetics, where alleles A and B exhibit codominance, while allele O is recessive. Consequently, the combination of alleles inherited from both parents dictates the child’s blood group, illustrating the concept of blood type inheritance similar to the inheritance of traits such as eye color.
Statistically, the distribution of blood groups varies across populations worldwide. For instance, group O negative is present in approximately 7% of the global population. Furthermore, Rh-negative blood groups, often referred to as ‘golden blood,’ are exceedingly rare, with only about fifty individuals recognized globally. This rarity underscores the importance of understanding blood type inheritance, especially in the context of genetic counseling, where accurate family history and genetic information are crucial for effective patient care.
Real-world examples further illustrate the complexities of blood type inheritance and ABO gene transmission within families. For example, if one parent has the A factor (genotype AA or AO) and the other has the B factor (genotype BB or BO), their offspring could potentially exhibit any of the four phenotypes, depending on the alleles inherited. This variability highlights the critical role of genetic counseling in elucidating the implications of blood group genetics for families.
Explore Genetic Mechanisms of Blood Type Inheritance
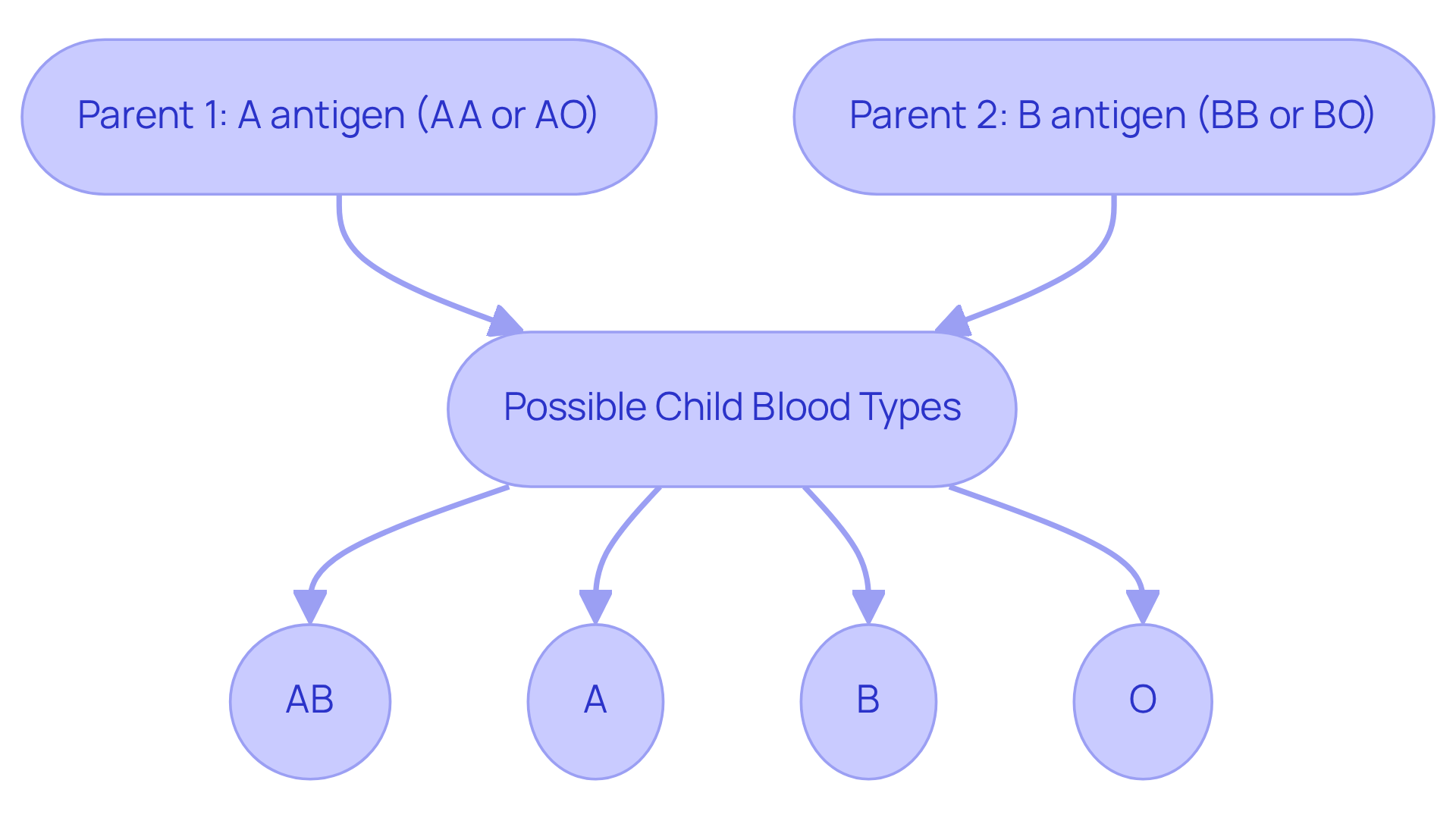
The genetic mechanisms governing fluid group inheritance are primarily dictated by the ABO gene located on chromosome 9. Each parent contributes one allele, resulting in a combination that determines the child’s phenotype. For instance, if one parent possesses the A antigen (genotype AA or AO) and the other has the B antigen (genotype BB or BO), their child may inherit one of the following combinations: AB, A, B, or O. The codominance of the A and B alleles allows for both to be expressed simultaneously, leading to the AB blood type. In contrast, the recessive O allele is only expressed when both inherited alleles are O. Understanding this genetic interaction is crucial for comprehending transfusion compatibility and blood type inheritance associated with the circulatory system. Recent advancements, such as the identification of the 48th type of serum system, known as Gwada-negative, underscore the evolving landscape of classification. Dr. Sarah Wilson notes, ‘The discovery of the MAL classification system is a remarkable accomplishment that will certainly have extensive effects on the future of medical care.’ Grasping these complexities is essential for genetic counselors, as accurate predictions of combination outcomes are vital for managing patient expectations and health outcomes.
Examine the Historical Context of Blood Type Discovery
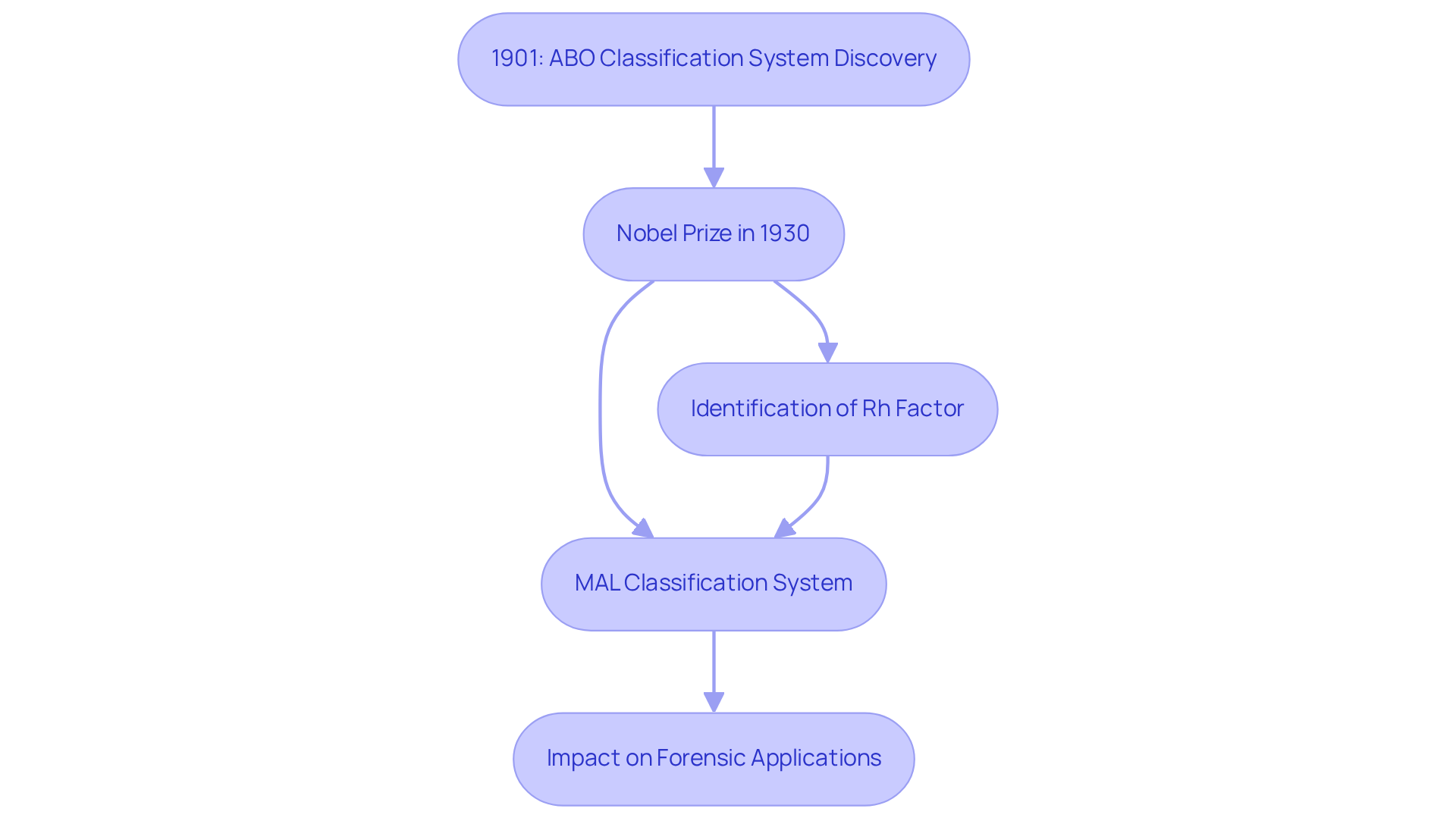
The classification of plasma varieties began in 1901 with Austrian doctor Karl Landsteiner’s discovery of the ABO classification system. This groundbreaking research demonstrated that plasma could be categorized based on specific antigens, a vital finding for ensuring safe transfusions. Landsteiner’s monumental achievement not only earned him the Nobel Prize in Physiology or Medicine in 1930 but also laid the foundation for modern immunology and transfusion medicine.
Subsequent research has expanded our understanding of circulatory fluid classifications, notably through the identification of the Rh factor and the MAL classification system. These advancements have significantly enhanced transfusion safety and patient management. The historical significance of these classifications continues to impact medical practices today, particularly in genetics and patient care. Understanding these classifications is crucial for effective healthcare delivery. As noted by Joan C. Stevenson, "Today, group classification is essential for a variety of applications, including health care and anthropological studies."
Furthermore, Landsteiner’s findings have paved the way for forensic applications, such as paternity testing, which gained legal recognition in the early 20th century.
Understand Medical Implications of Blood Type Inheritance
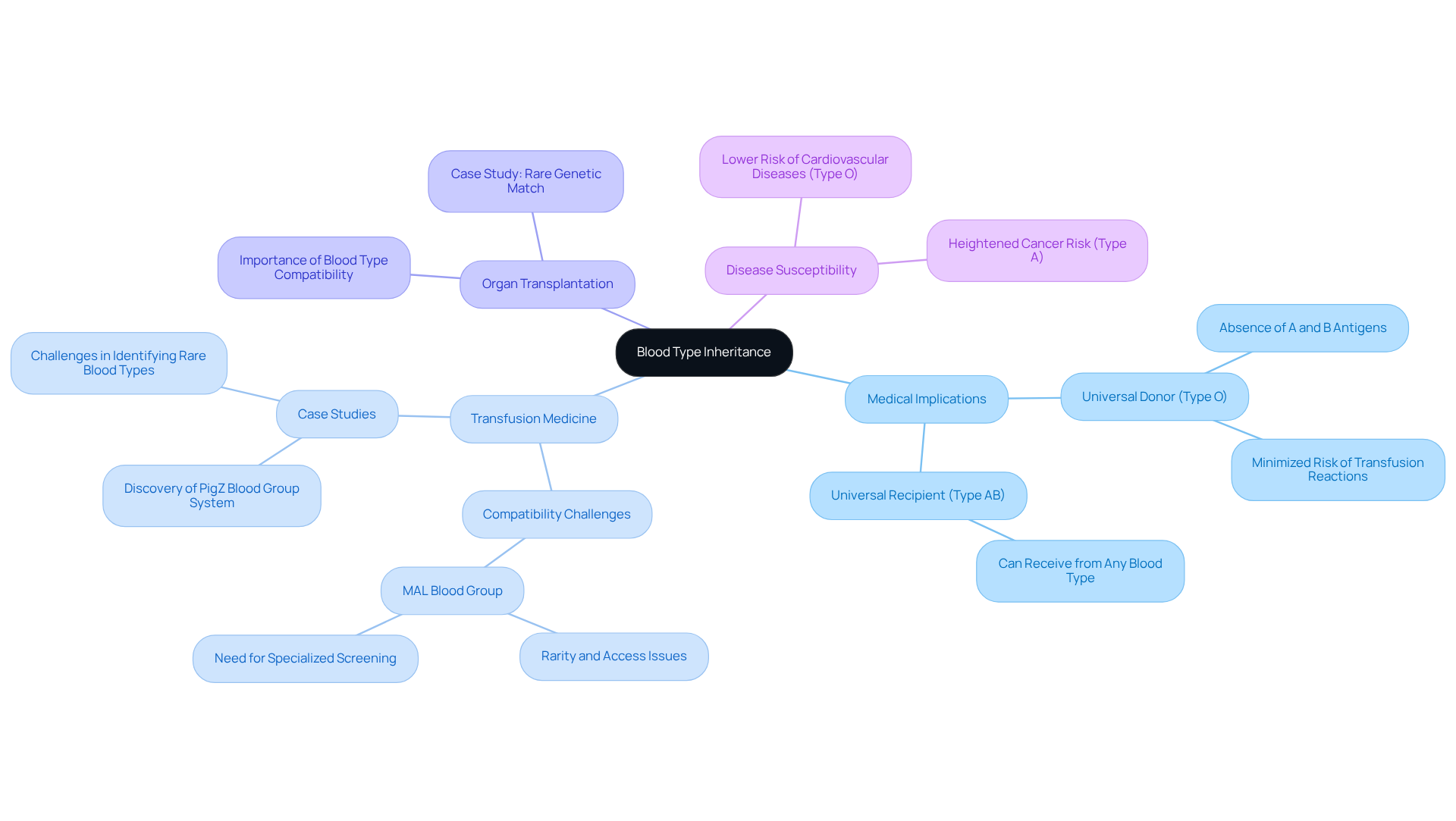
Blood group inheritance is crucial in medical practices, particularly in transfusion medicine, organ transplantation, and disease susceptibility. Approximately 45% of the population has O plasma, recognized as the universal donor type due to the absence of A and B antigens, which significantly minimizes the risk of transfusion reactions. Conversely, individuals with the AB group, making up about 4% of the population, can receive donations from any blood type, rendering them universal recipients.
Recent research indicates that blood groups may influence susceptibility to certain diseases. For example, individuals with the O group exhibit a lower risk of developing cardiovascular diseases, while those with the A group may face a heightened risk of specific cancers.
In organ transplantation, the compatibility of blood groups is paramount. A notable case involved a patient with a rare genetic match who faced challenges in finding a compatible donor. This highlights the significance of understanding blood type inheritance, since mismatched transfusions can result in severe immune reactions. The discovery of new circulatory type systems, such as the exceptionally rare MAL type, complicates this landscape further, emphasizing the necessity for specialized screening and management strategies. Individuals with the MAL group may encounter difficulties in accessing compatible supplies, necessitating targeted approaches in transfusion medicine.
Healthcare providers must consider blood type inheritance when making decisions regarding transfusions, pregnancy management, and genetic counseling, as it can significantly influence patient outcomes and treatment strategies.
Conclusione
Understanding blood type inheritance is crucial for comprehending how genetic traits are transmitted from parents to offspring. This process not only determines an individual’s blood group but also has significant implications for medical practices, genetic counseling, and health awareness. Through the lens of Mendelian genetics, it is clear that the combination of alleles from each parent dictates blood type, which can be classified as A, B, AB, or O, each with distinct characteristics and medical relevance.
The genetic mechanisms underlying blood type inheritance are explored, emphasizing the role of the ABO gene. Understanding these patterns is vital for ensuring transfusion compatibility and enhancing patient care. Historical insights highlight the pioneering work of Karl Landsteiner, whose discoveries established the foundation for modern transfusion medicine and genetics. Furthermore, the medical implications of blood type inheritance are critical, particularly in the context of transfusions, organ transplants, and disease susceptibility.
In conclusion, the importance of blood type inheritance transcends mere classification; it is a fundamental aspect of genetic understanding that can significantly influence health outcomes and patient management strategies. As advancements in genetic research progress, remaining informed about blood types and their implications will empower both individuals and healthcare professionals to make informed decisions that enhance patient care and safety. Embracing this knowledge enriches personal health awareness and fosters a more informed community capable of navigating the complexities of genetics and medicine.






