
Introduction
Hereditary lung disease represents a range of genetic conditions that can significantly impact respiratory health. Despite their potential severity, these diseases often remain underrecognized and misunderstood. Understanding the definitions, origins, and symptoms of these conditions is crucial, as it underscores the importance of early diagnosis and genetic testing. Such measures can lead to improved management and treatment options for affected individuals.
However, the complexities of inheritance patterns and the diverse manifestations of these conditions present challenges for individuals and families. To effectively navigate these challenges, it is essential to grasp the nuances of hereditary lung diseases and the implications they hold for respiratory health.
Define Hereditary Lung Disease
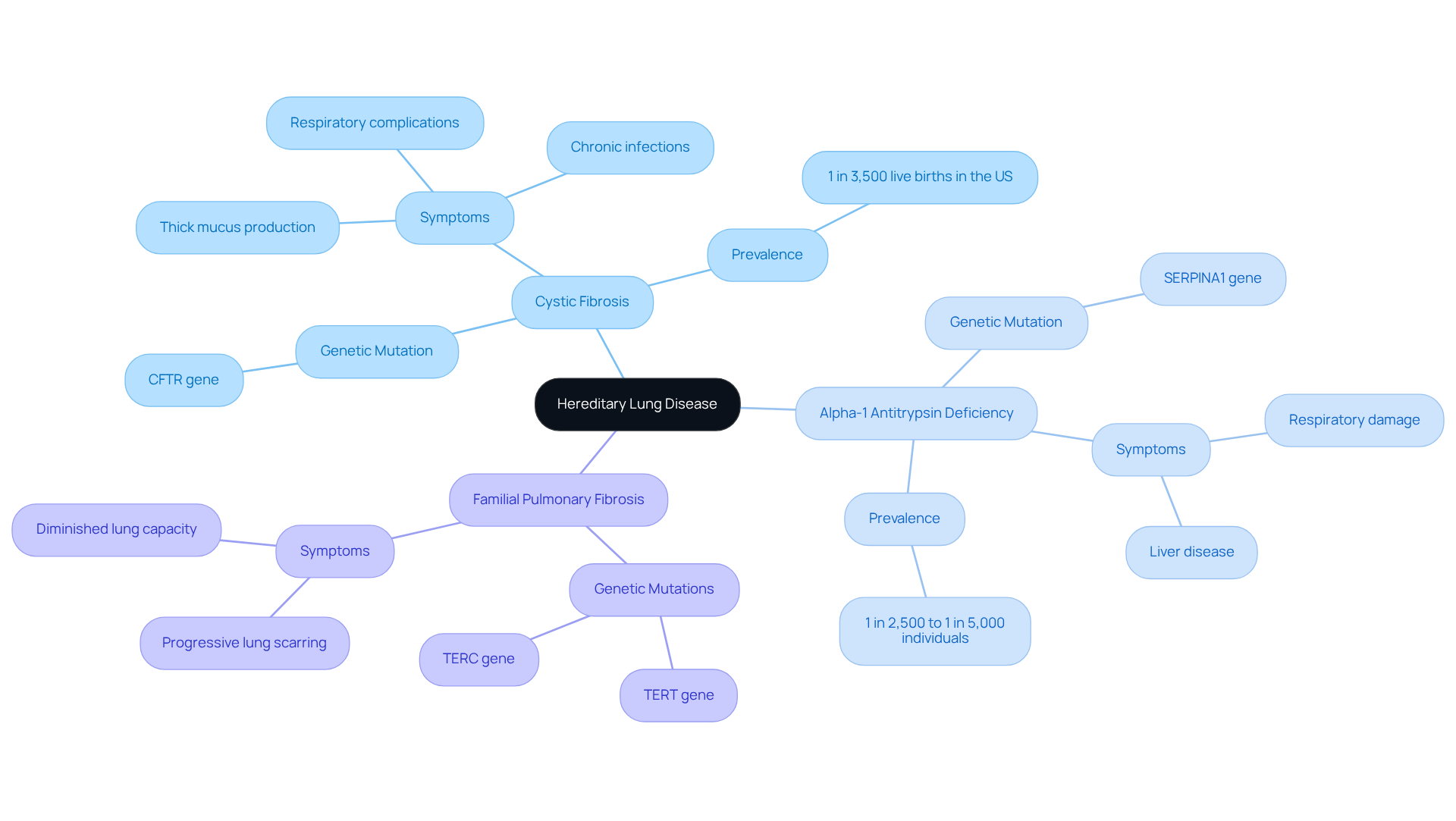
Hereditary lung disease includes a range of conditions transmitted through genetic mutations, which can significantly impair respiratory function and structure. Notable examples include:
- Cystic fibrosis, characterized by mutations in the CFTR gene, leading to thick mucus production and various respiratory complications.
- Alpha-1 antitrypsin deficiency, arising from mutations in the SERPINA1 gene, which can result in respiratory damage as well as liver disease.
- Familial pulmonary fibrosis, often associated with mutations in genes such as TERT and TERC, leading to progressive lung scarring and diminished lung capacity.
Statistics underscore the substantial impact of these conditions:
- Cystic fibrosis affects approximately 1 in 3,500 live births in the United States.
- The prevalence of alpha-1 antitrypsin deficiency varies widely, with estimates ranging from 1 in 2,500 to 1 in 5,000 individuals in specific populations.
Recent research highlights the importance of hereditary testing and counseling, as early diagnosis can facilitate improved management strategies and enhance patient outcomes.
Geneticists emphasize the necessity of awareness and understanding of inherited respiratory conditions, noting that “the detection of genetic mutations not only assists in diagnosis but also creates opportunities for targeted treatments.” As research advances, the focus on hereditary lung disease illustrates the critical intersection of genetics and respiratory health, underscoring the need for specialized medical management and support for individuals affected by this condition.
Context and Importance of Hereditary Lung Disease
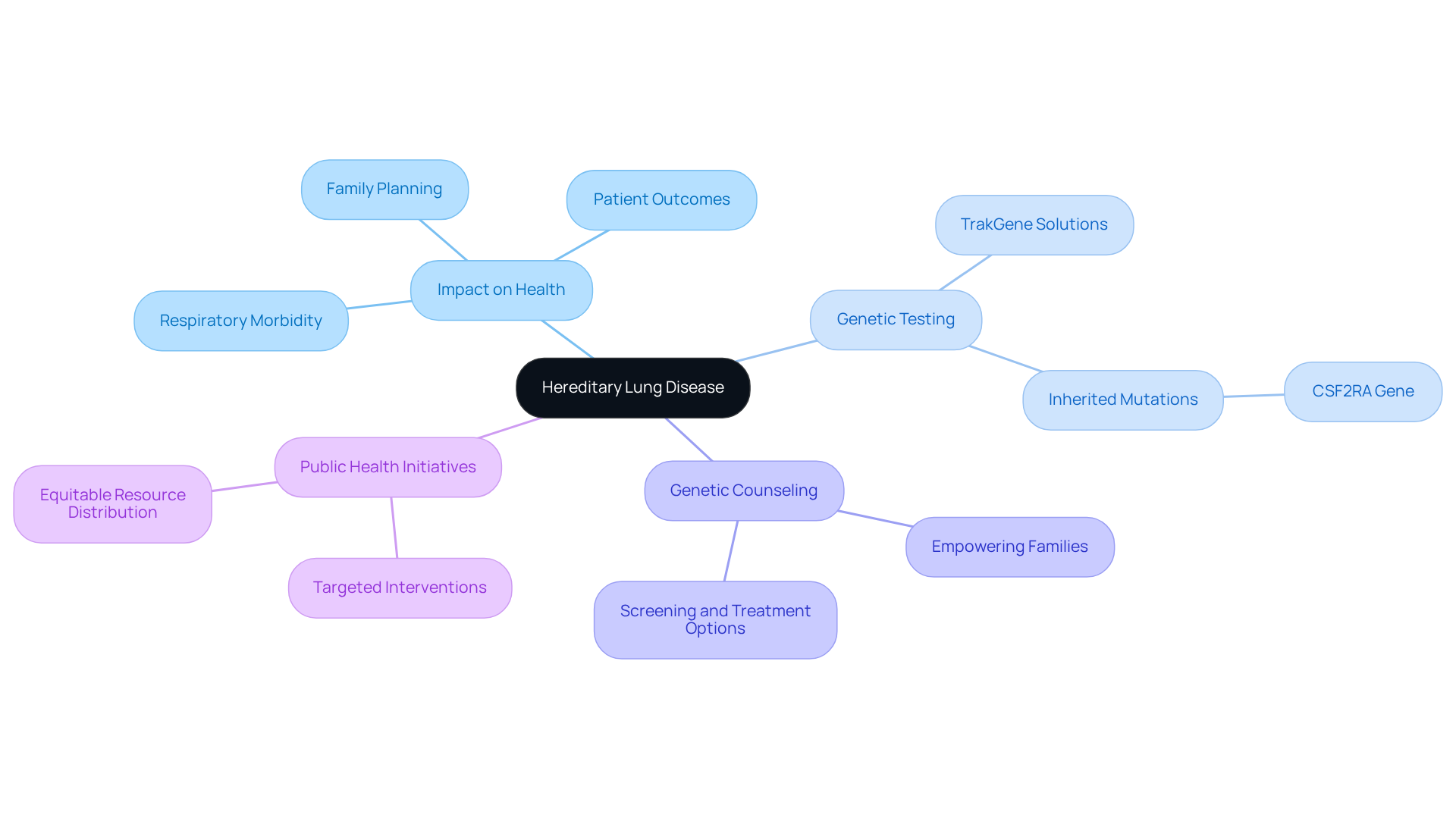
Hereditary lung disease is increasingly recognized as a significant contributor to respiratory morbidity and mortality. Recent advancements in genetic testing, particularly through TrakGene’s innovative digital solutions, have enhanced the diagnosis of these conditions, leading to more effective management strategies. In 2021, approximately 468.3 million people worldwide were affected by chronic respiratory conditions (CRCs), underscoring the urgent need for targeted public health measures and equitable healthcare resource distribution, especially in low- and middle-SDI areas.
The implications of hereditary lung disease extend beyond individual health, impacting family planning and public health initiatives. Genetic counseling is crucial in this context, empowering families to understand their risks and make informed decisions regarding screening and treatment options. TrakGene’s user-friendly pedigree chart tool facilitates the gathering of family history, which is essential for advisors managing conditions like chronic obstructive pulmonary disease (COPD) and pulmonary alveolar proteinosis (PAP), where hereditary factors play a significant role.
As research continues to uncover the foundations of hereditary lung disease in these conditions, it opens avenues for targeted treatments and improved patient outcomes. For example, identifying inherited mutations in the GM-CSF receptor alpha chain gene (CSF2RA) has been instrumental in understanding PAP, leading to novel diagnostic tests and potential therapies. The integration of genetic knowledge into clinical practice, supported by TrakGene’s advanced pedigree chart tool and enhanced data protection measures, not only improves personal care but also informs broader public health strategies aimed at reducing the impact of hereditary lung disease.
Origins and Genetic Mechanisms
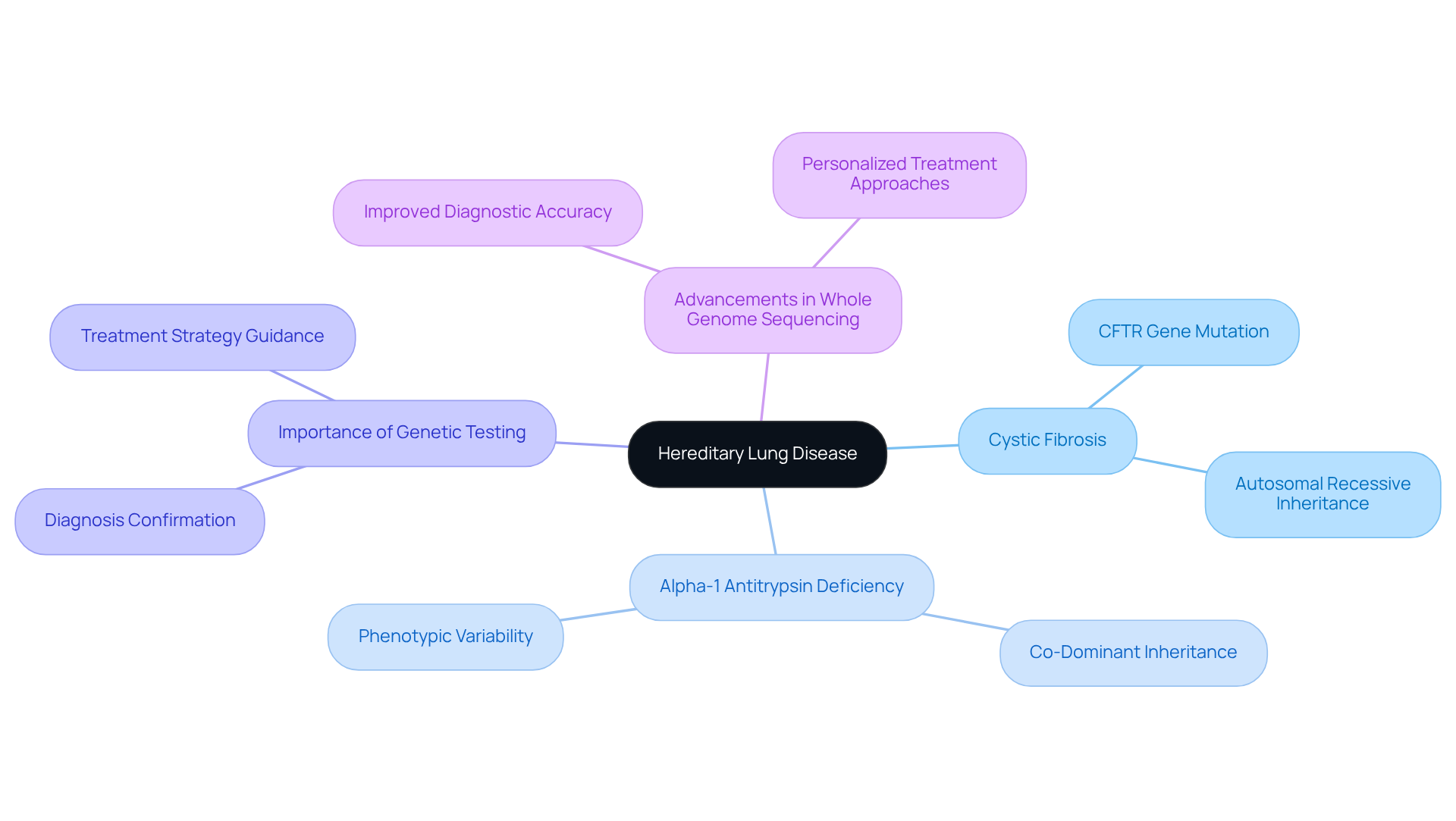
Hereditary lung disease is primarily caused by mutations in specific genes, which are inherited through patterns such as autosomal dominant, autosomal recessive, or X-linked inheritance. For example, cystic fibrosis results from mutations in the CFTR gene and follows an autosomal recessive inheritance pattern. This means that an individual must inherit two copies of the mutated gene to exhibit the disease. In contrast, alpha-1 antitrypsin deficiency is inherited in an autosomal co-dominant manner, where both alleles contribute to the phenotype, resulting in varying degrees of deficiency among individuals.
Understanding the mechanisms of hereditary lung disease is crucial for identifying at-risk individuals and facilitating early interventions. Recent studies have highlighted the significance of specific CFTR gene mutations in the severity of respiratory conditions, underscoring the need for targeted genetic testing. Genetic testing not only confirms diagnoses but also informs treatment strategies, making it an essential tool in managing hereditary lung disease.
Advancements in whole genome sequencing have notably improved diagnostic accuracy, enabling the identification of previously undiagnosed cases and allowing for personalized treatment approaches.
Key Characteristics and Symptoms
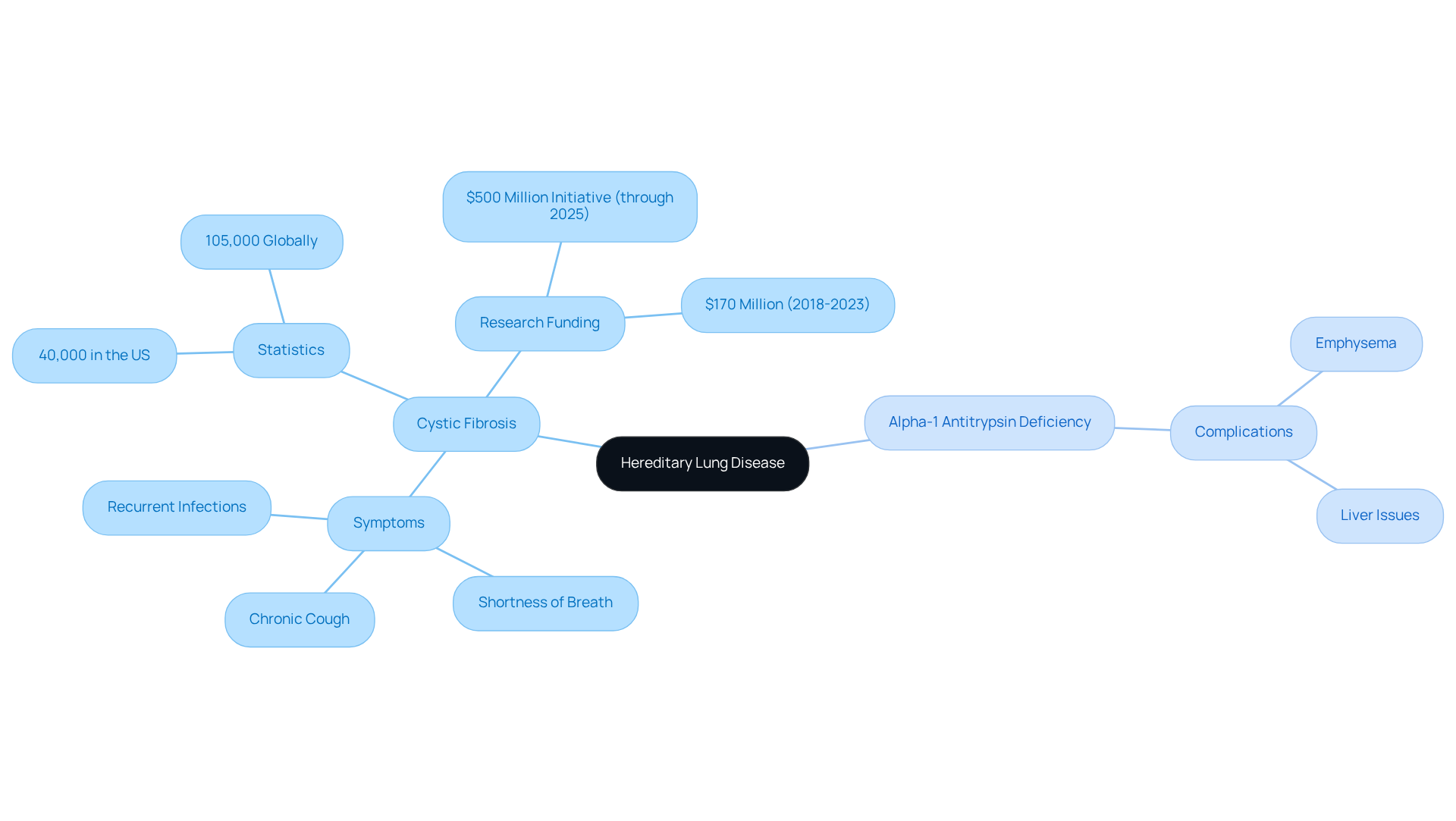
Hereditary lung disease presents a variety of characteristics, including common symptoms such as chronic cough, shortness of breath, and recurrent respiratory infections. Cystic fibrosis (CF) exemplifies this, characterized by the production of thick, sticky mucus that obstructs airways, resulting in frequent lung infections and progressive loss of lung function. In the United States, approximately 40,000 individuals are affected by CF, with an estimated 105,000 diagnosed globally.
The CF Foundation has committed over $170 million from 2018 to 2023 towards research and development of new treatments, underscoring ongoing efforts to enhance patient outcomes. Furthermore, the Path to a Cure initiative aims to allocate $500 million through 2025 to expedite CF drug discovery and development.
In contrast, alpha-1 antitrypsin deficiency can lead to emphysema and liver complications due to the buildup of abnormal proteins in the body. The CF Foundation accredits over 130 care centers staffed by healthcare professionals, ensuring expert care for individuals with CF.
Early recognition of symptoms is crucial, as timely diagnosis and intervention can significantly improve patient outcomes and enhance quality of life. For instance, advancements in CF treatment have led to the approval of more than twelve new therapies, highlighting the importance of early detection and management in hereditary lung disease. As Katie K., an adult with CF, noted, the journey to diagnosis can be challenging; however, understanding the disease is essential for effective management.
Conclusion
Addressing hereditary lung diseases is of paramount importance. As advancements in genetic research continue to unfold, there exists a significant opportunity for enhanced public health initiatives and equitable healthcare access. Individuals, families, and healthcare providers must remain informed about the implications of these conditions, fostering a proactive approach to diagnosis and management. Engaging with resources such as genetic counseling and testing can profoundly impact the quality of life for those affected, making awareness and education essential in the fight against hereditary lung disease.
Hereditary lung disease represents a complex interplay of genetic factors that can profoundly impact respiratory health. Understanding the definitions, origins, and symptoms of these conditions enables individuals to navigate the challenges they present more effectively. This knowledge is crucial not only for those affected but also for healthcare professionals and families, as it lays the groundwork for informed decision-making and effective management strategies.
The article highlights significant hereditary lung diseases, including:
- Cystic fibrosis
- Alpha-1 antitrypsin deficiency
- Familial pulmonary fibrosis
Each condition is associated with specific genetic mutations that dictate inheritance patterns and clinical manifestations. The importance of early diagnosis and genetic testing is underscored, as these tools can lead to improved patient outcomes and the development of targeted therapies. Furthermore, the role of genetic counseling is vital in empowering families to understand their risks and make informed choices regarding health and family planning.
Frequently Asked Questions
What is hereditary lung disease?
Hereditary lung disease refers to a range of conditions passed down through genetic mutations that can severely affect respiratory function and structure.
What are some examples of hereditary lung diseases?
Notable examples include cystic fibrosis, alpha-1 antitrypsin deficiency, and familial pulmonary fibrosis.
How does cystic fibrosis affect the body?
Cystic fibrosis is characterized by mutations in the CFTR gene, leading to the production of thick mucus, which can cause various respiratory complications.
What causes alpha-1 antitrypsin deficiency?
Alpha-1 antitrypsin deficiency arises from mutations in the SERPINA1 gene, resulting in potential respiratory damage as well as liver disease.
What are the implications of familial pulmonary fibrosis?
Familial pulmonary fibrosis is often linked to mutations in genes like TERT and TERC, leading to progressive lung scarring and reduced lung capacity.
What are the prevalence statistics for these conditions?
Cystic fibrosis affects approximately 1 in 3,500 live births in the United States, while alpha-1 antitrypsin deficiency varies in prevalence from 1 in 2,500 to 1 in 5,000 individuals in certain populations.
Why is hereditary testing and counseling important?
Hereditary testing and counseling are crucial because early diagnosis can lead to better management strategies and improved patient outcomes.
What do geneticists say about the detection of genetic mutations in hereditary lung diseases?
Geneticists emphasize that detecting genetic mutations assists in diagnosis and creates opportunities for targeted treatments, highlighting the intersection of genetics and respiratory health.






