
Einführung
Understanding hereditary diseases is essential for genetic counselors as they navigate the complexities of patient care and family planning. This article explores ten key examples of hereditary diseases, emphasizing their genetic foundations and the critical role of genetic counseling in managing these conditions. With the continuous evolution of genetic technology, counselors must consider how to effectively utilize these tools to improve patient outcomes while addressing the emotional and logistical challenges that families encounter.
TrakGene: Advanced Solutions for Managing Hereditary Diseases
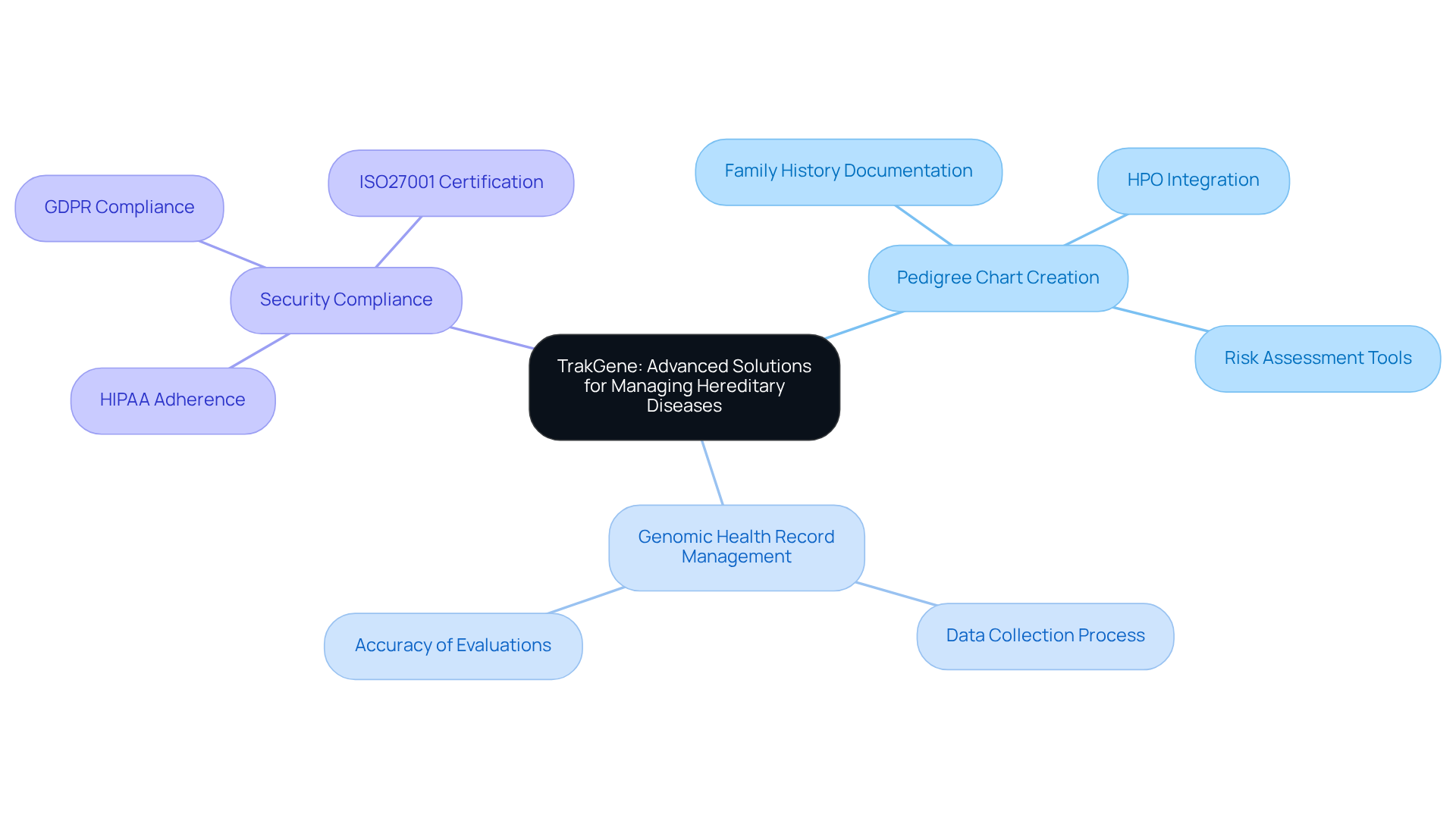
TrakGene offers advanced digital solutions specifically designed for genetics professionals, emphasizing pedigree chart creation and genomic health record management. Their innovative pedigree chart maker facilitates comprehensive family history documentation, seamlessly integrating Human Phenotype Ontology (HPO) terms and risk assessment tools.
Genetic advisors have noted that these sophisticated tools not only streamline the data collection process but also enhance the accuracy of evaluations related to examples of hereditary diseases. This improvement leads to more informed healthcare decisions for patients, allowing hereditary specialists to efficiently gather and analyze examples of hereditary diseases. As a result, patient care and clinical outcomes are significantly improved.
TrakGene’s commitment to security is evident in its adherence to HIPAA and GDPR standards, alongside the implementation of an ISO27001 Information Security Management System. This dedication further solidifies its reputation as a trustworthy partner in the oversight of genetic data.
Sickle Cell Disease: Genetic Basis and Implications
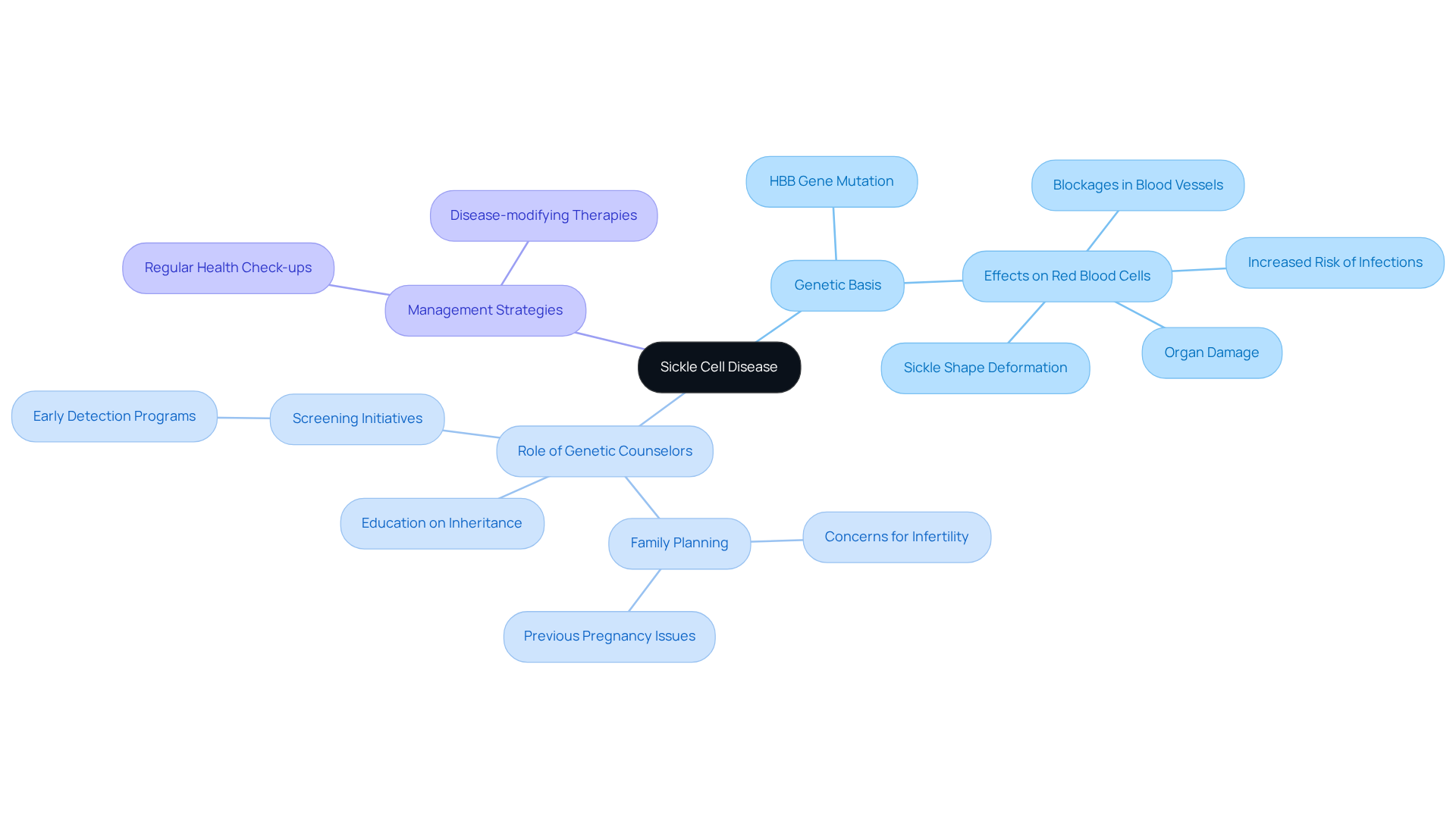
Sickle Cell Disease (SCD) is caused by a mutation in the HBB gene, leading to the production of abnormal hemoglobin that distorts red blood cells into a sickle shape. This deformation results in blockages in blood vessels, which can cause severe pain and a variety of complications, including an increased risk of infections and organ damage.
Genetic counselors play a vital role in this context by educating families about inheritance patterns. It is important to note that approximately 1 in 13 Black or African-American children carry one copy of the sickle cell mutation. Counselors also guide families through the complexities of SCD management strategies, which encompass pain management techniques and preventive care measures.
For instance, hereditary counseling can address concerns regarding family planning, particularly for individuals with a history of infertility or previous pregnancies affected by examples of hereditary diseases. Additionally, hereditary advisors can facilitate access to screening initiatives that detect SCD early, allowing for timely interventions that significantly improve quality of life.
Current management strategies underscore the necessity of comprehensive care, which includes:
- Regular health check-ups
- Implementation of disease-modifying therapies
These approaches can help alleviate the complications associated with SCD. As advancements in hereditary therapies continue to evolve, the role of advisors will also adapt, ensuring that patients and their families remain well-informed and supported throughout their healthcare journey.
Cystic Fibrosis: Understanding Its Genetic Mechanism
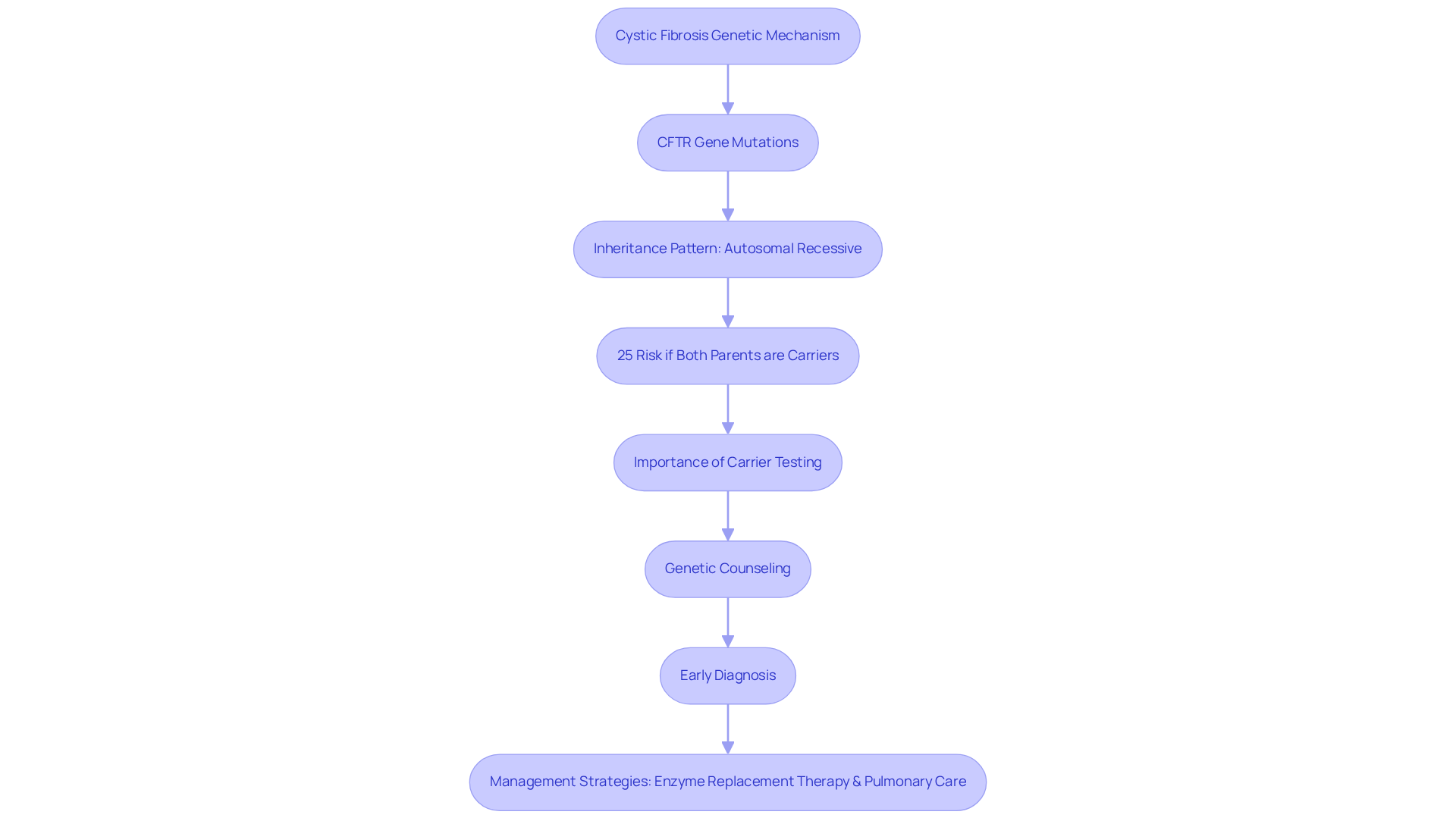
Cystic Fibrosis (CF) is an autosomal recessive disorder caused by mutations in the CFTR gene, which is essential for regulating salt and water transport across cell membranes. This dysfunction leads to the accumulation of thick mucus in various organs, particularly impacting the lungs and pancreas. Understanding the inheritance pattern is crucial; both biological parents must be carriers for a child to inherit CF, resulting in a 25% risk of the condition if both parents carry the gene mutation. Genetic advisors are instrumental in informing relatives about carrier testing, which is essential for making informed reproductive decisions.
Early diagnosis is vital, as timely intervention can significantly enhance health outcomes. The Cystic Fibrosis Foundation recommends comprehensive screening for as many CF-causing variants as possible. Some states only test for the most common mutations, which may overlook cases in underrepresented populations. For example, while the delta F508 variant is prevalent, over 1,700 mutations can cause CF, underscoring the necessity for thorough genetic testing.
Management strategies for CF include enzyme replacement therapy to assist digestion and pulmonary care to address respiratory issues. These approaches are critical for improving the quality of life and longevity of individuals with CF, as advancements in treatment have enabled many to live into their 40s and beyond. Genetic counselors must emphasize the importance of early diagnosis and ongoing management to families, ensuring they are equipped with the knowledge to navigate this complex condition.
Huntington’s Disease: Genetic Inheritance and Symptoms
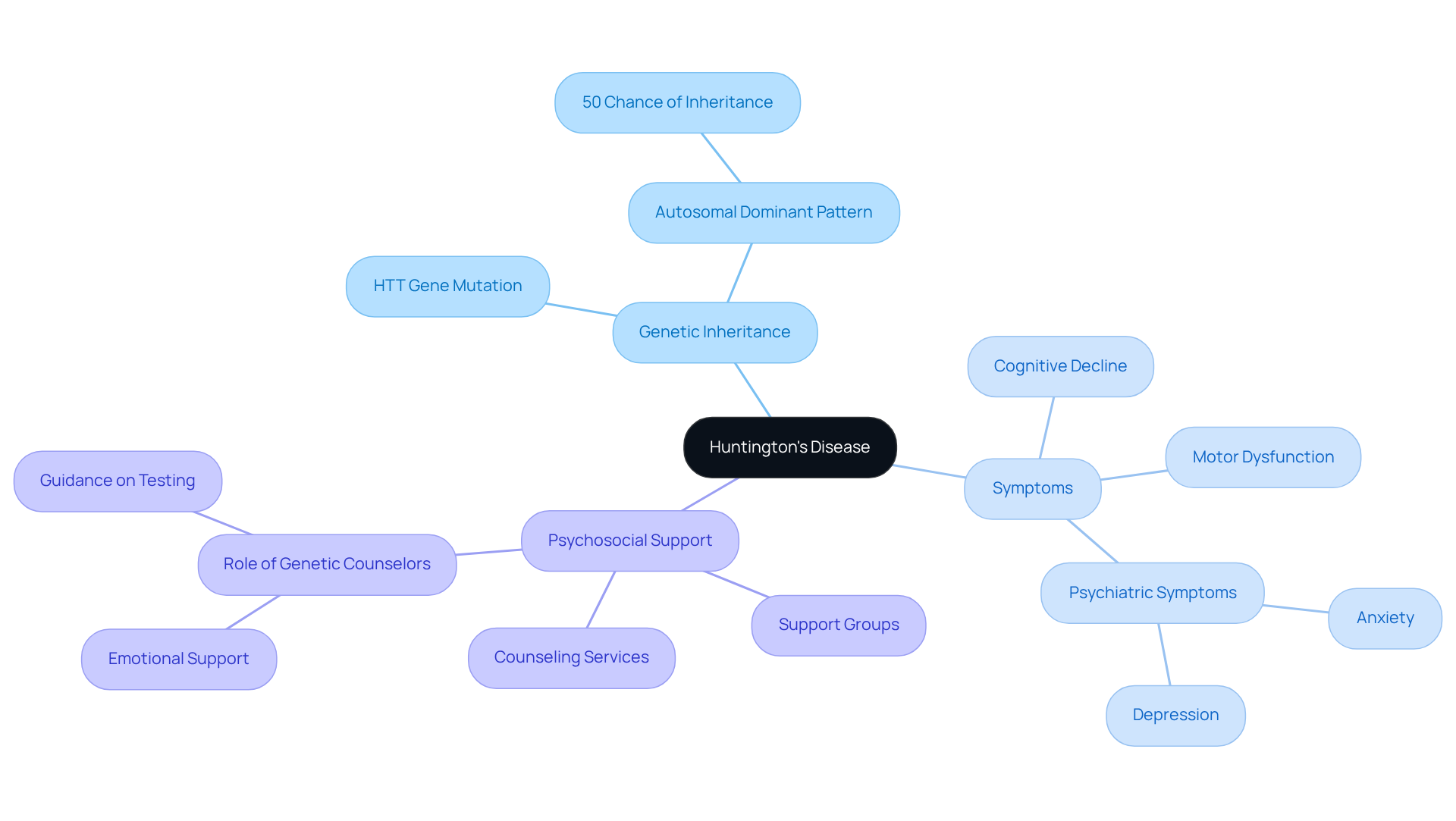
Huntington’s Disease (HD) is one of the examples of hereditary diseases, as it is a hereditary neurodegenerative disorder caused by a mutation in the HTT gene. It is characterized by progressive motor dysfunction, cognitive decline, and psychiatric symptoms. Huntington’s disease (HD) is one of the examples of hereditary diseases that follows an autosomal dominant inheritance pattern, meaning that each child of an affected parent has a 50% chance of inheriting the mutation. Symptoms typically manifest in mid-adulthood, often between the ages of 30 and 50, but can appear earlier or later in life.
The psychosocial effect of HD on households is profound. Individuals diagnosed with HD often encounter emotional difficulties, such as anxiety and depression, which can significantly impact their quality of life and that of their relatives. Genetic counselors play a crucial role in supporting individuals through the complexities of testing and the implications of a positive diagnosis. They provide guidance on managing the emotional and practical aspects of living with HD, emphasizing the importance of open communication and support networks.
Recent findings indicate that the prevalence of HD varies significantly across regions, with higher rates observed in Europe and North America compared to Africa and Asia. For instance, the prevalence of HD in Scotland is reported at 15.00 per 100,000, while Finland shows a prevalence of 2.12 per 100,000. The pooled incidence of HD is estimated at 0.48 cases per 100,000 person-years, with a prevalence of 4.88 per 100,000. This variability underscores the need for tailored psychosocial support that considers cultural and regional differences in healthcare access and stigma surrounding genetic conditions.
Real-world examples of psychosocial support include support groups and counseling services that help families navigate the emotional landscape of HD. Genetic advisors highlight the significance of these resources, stating that they can greatly ease feelings of isolation and anxiety. As counselor Nick noted, “Some individuals who chose to undergo testing do so to assist them in planning what they would like to do with their life.” Comprehending the psychosocial aspects of Huntington’s Disease is crucial for delivering comprehensive care to those impacted.
Furthermore, progress in DNA testing has changed the environment for households at risk. With improved access to testing, households can make informed decisions about their health and future. However, the choice to undergo testing for examples of hereditary diseases can be fraught with emotional challenges, as individuals weigh the potential benefits against the psychological burden of knowing their status. Genetic advisors are essential in assisting households navigate these decisions, ensuring they have the support necessary to manage the consequences of their choices. Notably, de novo mutations account for an estimated 7.1% of new HD cases, adding another layer of complexity to the genetic discussion surrounding HD.
Hemophilia: Genetic Factors and Treatment Options
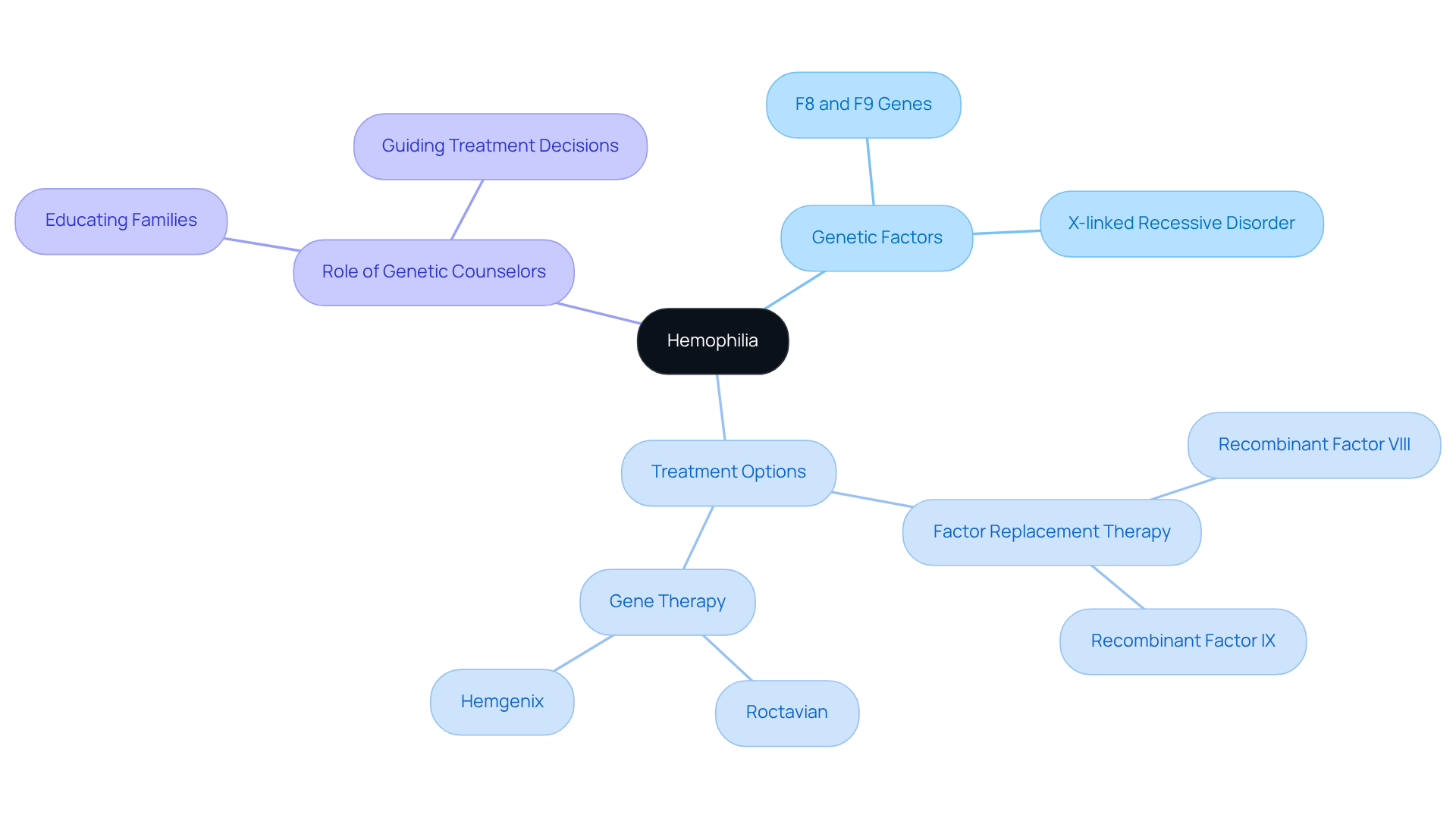
Hemophilia is an X-linked recessive disorder caused by mutations in the F8 or F9 genes, leading to deficiencies in clotting factors. This condition results in prolonged bleeding episodes, which can lead to serious complications, including life-threatening brain bleeds and organ damage. Genetic counselors play a vital role in educating families about inheritance patterns, potential complications, and treatment options, such as factor replacement therapy and advancements in gene therapy.
Factor replacement therapy is a cornerstone of hemophilia management. This therapy involves administering clotting factors to prevent or control bleeding episodes. For example, recombinant factor VIII and IX concentrates, which do not contain human plasma, are widely used and have been shown to significantly reduce bleeding frequency. Approximately 75 percent of hemophilia patients utilize these recombinant products, underscoring their effectiveness in treatment.
Recent advancements in gene therapy have transformed the landscape of hemophilia care. The FDA-approved gene therapies, including Roctavian for severe hemophilia A (approved on June 29, 2023) and Hemgenix for hemophilia B (approved on November 22, 2022), offer promising alternatives by enabling patients to produce their own clotting factors. These therapies have demonstrated the potential to significantly reduce bleeding episodes, thereby improving the quality of life for many patients. However, it is important to note that only about 15 percent of the global population has access to effective treatment for hemophilia, highlighting the critical role of genetic counseling.
Genetic advisors emphasize the importance of informing relatives about these treatment possibilities. As one advisor stated, “Grasping the progress in hemophilia treatment enables households to make educated choices regarding their care, particularly when they discover how these alternatives can greatly affect their loved ones’ lives.”
In summary, the incorporation of factor replacement treatments and novel gene therapies signifies a considerable advance in managing hemophilia, underscoring the crucial role of specialists in assisting families through these complex decisions. Comprehensive hemophilia treatment centers (HTCs) also play a vital role in providing specialized care and support for individuals with hemophilia.
Marfan Syndrome: Genetic Characteristics and Health Risks
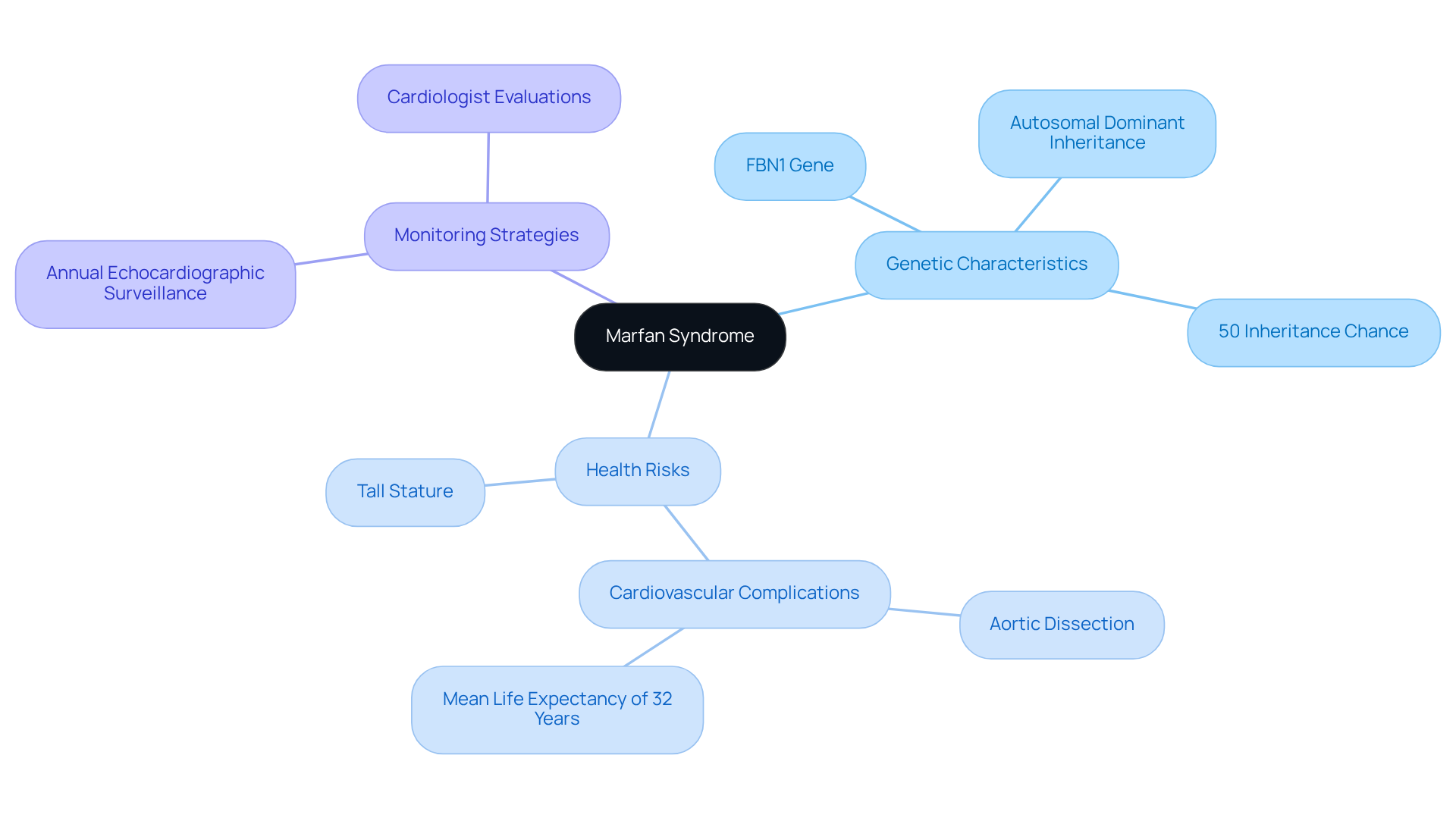
Marfan Syndrome is an autosomal dominant disorder caused by mutations in the FBN1 gene, which is essential for maintaining connective tissue integrity. This condition is characterized by features such as tall stature, elongated limbs, and significant cardiovascular complications, necessitating vigilant monitoring.
Each child of an affected parent has a 50% chance of inheriting the disorder, which underscores the importance of genetic counseling for families with examples of hereditary diseases. Statistics indicate that untreated individuals with Marfan Syndrome have a mean life expectancy of only 32 years, primarily due to cardiovascular issues, which are responsible for the majority of premature deaths in this population. The leading cause of death in classical Marfan syndrome is aortic dissection or rupture.
Regular cardiovascular monitoring is crucial; studies show that 60-85% of individuals with classical Marfan Syndrome experience aortic dilation, with severe cases potentially leading to life-threatening conditions such as aortic dissection. Notably, aortic dilation occurs in 80-100% of early-onset Marfan syndrome cases. Real-world examples emphasize the necessity of annual echocardiographic surveillance, especially when the aortic root diameter exceeds 4.5 cm. More frequent evaluations by a cardiologist are warranted when the aortic root diameter surpasses this threshold.
Genetic advisors play a vital role in educating relatives about these risks and the importance of proactive health management to mitigate complications associated with Marfan Syndrome.
Tay-Sachs Disease: Genetic Causes and Consequences
Tay-Sachs Disease Overview
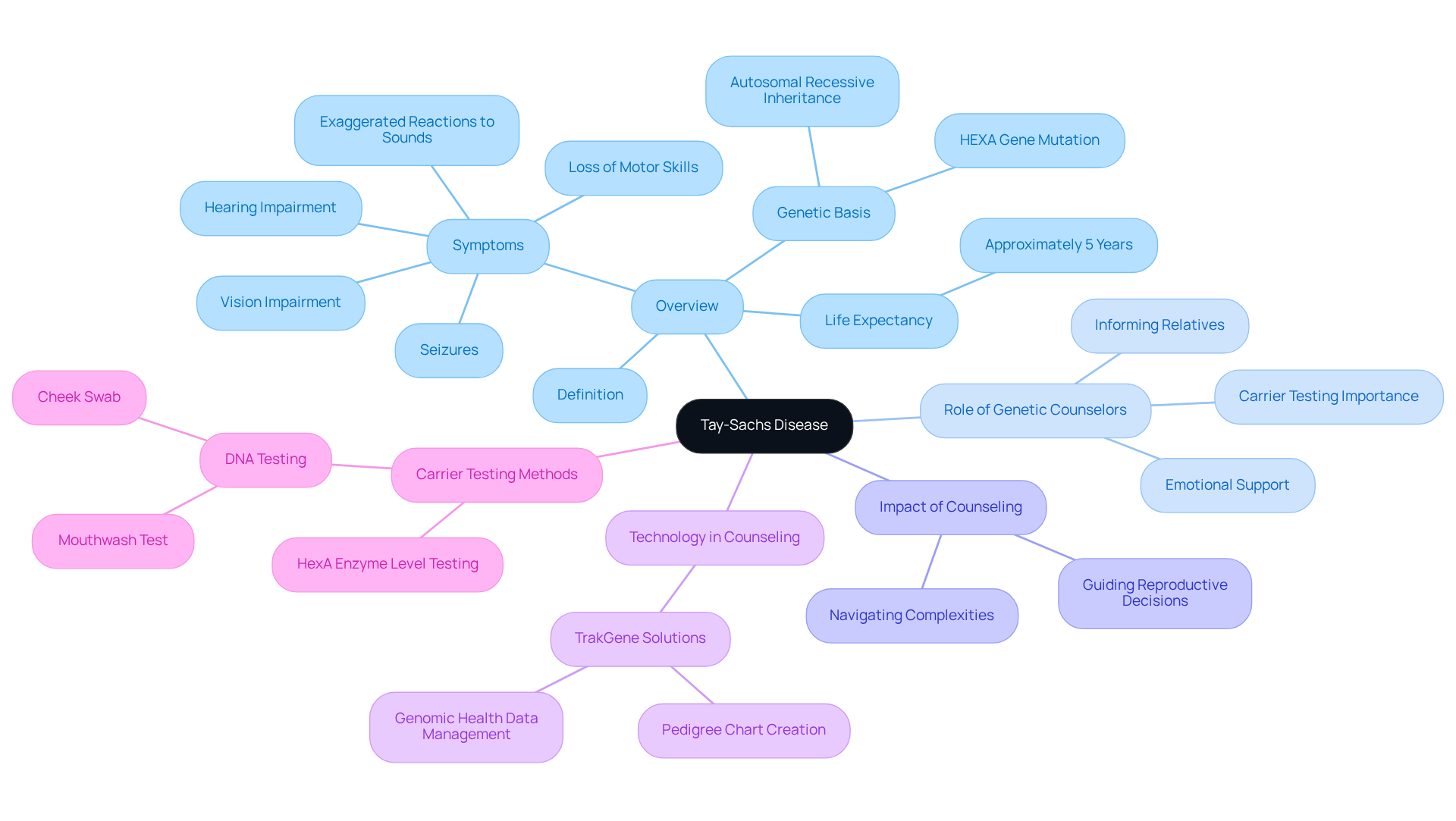
Tay-Sachs Disease (TSD) is an autosomal recessive disorder caused by mutations in the HEXA gene, leading to the accumulation of GM2 gangliosides in the brain. This accumulation results in progressive neurological decline, with symptoms typically appearing around six months of age. Affected children may experience loss of motor skills, vision and hearing impairment, and exaggerated reactions to sounds. The life expectancy for these children is approximately five years, underscoring the critical need for early diagnosis and intervention.
Role of Genetic Counselors
Genetic counselors play a vital role in informing relatives about the inheritance pattern of TSD, which requires both parents to be carriers for a child to be affected. In high-risk populations, such as individuals of Ashkenazi Jewish or French-Canadian descent, the prevalence of carrier status is significantly higher, which makes carrier testing essential for identifying examples of hereditary diseases. For instance, if both parents are carriers, there is a 25% chance their child will inherit the disease, a 50% chance of being a carrier, and a 25% chance of being unaffected.
Impact of Genetic Counseling
Real-world examples illustrate the impact of genetic counseling in these communities. Counselors provide emotional assistance and details regarding testing alternatives, aiding individuals in navigating the complexities of TSD. They emphasize the significance of carrier testing, which can guide reproductive decisions and health care. As one hereditary advisor remarked, ‘Comprehending carrier status is essential for planning households and evaluating the risk of transmitting examples of hereditary diseases, including Tay-Sachs disease.’
Enhancing Counseling with Technology
TrakGene’s digital solutions can enhance the genetic counseling process by providing tools for effective pedigree chart creation and genomic health data management. These tools assist counselors in tracking histories related to Tay-Sachs disease, ensuring that households receive comprehensive support and information.
Carrier Testing Methods
Carrier testing for Tay-Sachs disease can involve checking HexA enzyme levels in the blood or examining DNA through non-invasive methods such as a mouthwash test or cheek swab. This proactive approach not only aids in early identification but also empowers households to make informed choices concerning their health and future offspring. The integration of genetic counseling and carrier testing, supported by TrakGene’s advanced tools, significantly enhances outcomes for households impacted by Tay-Sachs disease, fostering awareness and understanding in high-risk populations while ensuring compliance with data protection standards.
Phenylketonuria (PKU): Genetic Testing and Management
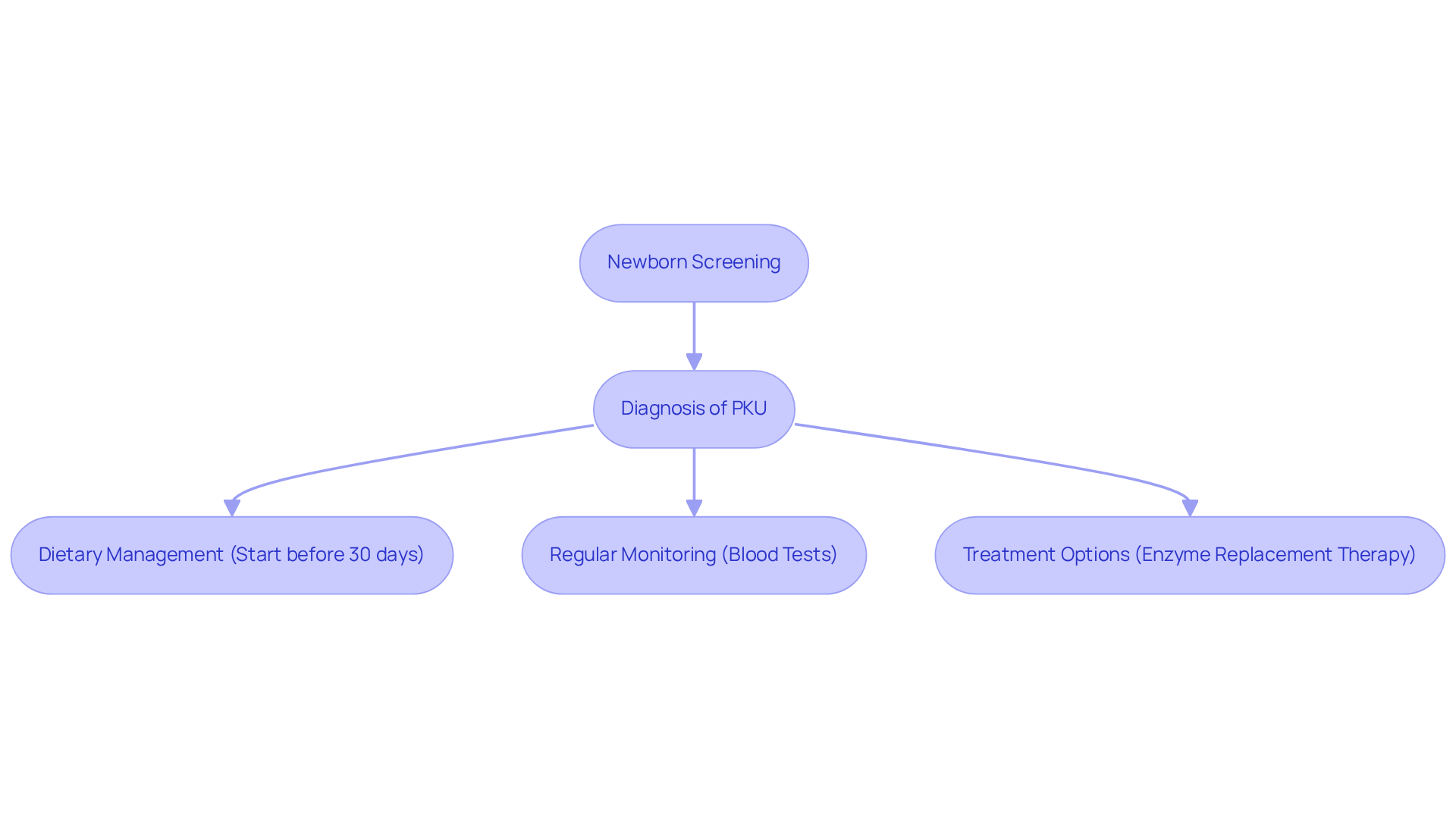
Phenylketonuria (PKU) is an autosomal recessive disorder caused by mutations in the PAH gene, which hinders the body’s ability to metabolize phenylalanine, an amino acid prevalent in many protein-rich foods. Early diagnosis through newborn screening is crucial, as untreated PKU can result in severe intellectual disabilities and developmental delays. Notably, newborn screening programs have successfully identified PKU in approximately 1 in 10,000 births, facilitating timely intervention.
Genetic counselors are vital in guiding families through the complexities of managing PKU. They stress the necessity of adhering to a strict low-phenylalanine diet, which should commence before the child reaches 30 days of age to avert irreversible cognitive impairment. Regular monitoring of phenylalanine levels through blood tests is essential to ensure the effectiveness of dietary restrictions and to modify treatment plans as needed.
Counselors also educate families about potential treatment options, including enzyme replacement therapy, which has shown promise in alleviating PKU symptoms. A collaborative approach involving healthcare providers, dietitians, and support networks is critical for the successful long-term management of the condition. As one hereditary advisor noted, “Effective management of PKU, an example of hereditary diseases, requires collaboration from all who interact with the child, including family, neighbors, friends, and educators.” This comprehensive support system not only aids in dietary compliance but also enables children with PKU to lead fulfilling lives despite their dietary limitations.
Achondroplasia: Genetic Basis and Clinical Features
Achondroplasia is an autosomal dominant disorder caused by mutations in the FGFR3 gene, which leads to impaired bone growth and results in dwarfism. Genetic counselors play a crucial role in providing families with essential information regarding the inheritance pattern, potential health risks, and the importance of early intervention and management strategies to address associated complications.
In this context, TrakGene offers advanced digital solutions that enhance the genetic counseling process. Our tools, including detailed pedigree charts and comprehensive genomic health records, facilitate the secure management of sensitive hereditary information. This capability is vital for ensuring that families receive accurate and timely guidance.
Moreover, our commitment to data protection is paramount. We adhere to HIPAA and GDPR standards, supported by our ISO27001 Information Security Management System. This underscores the importance of safeguarding patient data in genetic counseling, ensuring that sensitive information is handled with the utmost care and security.
Duchenne Muscular Dystrophy: Genetic Causes and Impact
Duchenne Muscular Dystrophy (DMD) is an X-linked recessive disorder caused by mutations in the DMD gene, which encodes the dystrophin protein crucial for maintaining muscle integrity. This condition results in progressive muscle degeneration, significantly affecting mobility and overall health.
Genetic advisors play a critical role in guiding families through the complexities of DMD, emphasizing the importance of understanding its inheritance pattern. Approximately 1 in every 5,000 males is diagnosed with DMD, with a median age of diagnosis around 5 years. Early diagnosis is essential, as it enables timely interventions such as physical therapy and emerging gene therapies, which can enhance quality of life and prolong mobility.
For example, boys who initiate steroid treatment at an early age may experience a delay in the loss of ambulation. Those who undergo steroid therapy for less than three years typically stop walking around age 9.5, whereas those who are treated for over five years may maintain ambulation until around age 12. Genetic counselors emphasize that proactive management strategies can significantly influence the disease’s progression.
Experts highlight that early identification of carriers and affected individuals is vital for informed family planning and risk assessment. This knowledge equips families to navigate the challenges associated with DMD effectively.
Abschluss
Understanding hereditary diseases is crucial for genetic counselors, as these conditions have a profound impact on individuals and families. This article emphasizes the significance of genetic counseling through ten key examples of hereditary diseases, illustrating the intricate relationship between genetic factors, inheritance patterns, and the essential role of genetic counseling in managing these conditions.
Each disease discussed, including:
- Sickle Cell Disease
- Cystic Fibrosis
- Huntington’s Disease
- Duchenne Muscular Dystrophy
highlights the necessity of early diagnosis and effective management strategies. Genetic counselors provide vital support, offering crucial information about inheritance patterns and guiding families through the emotional and practical implications of these diseases. Furthermore, advancements in technology, such as those offered by TrakGene, enhance the ability of genetic counselors to deliver comprehensive care and support.
The importance of genetic counseling cannot be overstated. As hereditary diseases continue to present challenges, the integration of advanced digital tools and thorough education empowers families to make informed health decisions. By fostering awareness and understanding, individuals can navigate the complexities of hereditary diseases more effectively, ultimately leading to improved outcomes and enhanced quality of life. Prioritizing genetic counseling and embracing these advancements is essential for anyone affected by hereditary conditions, ensuring they receive the necessary support and resources for effective management.
Häufig gestellte Fragen
What solutions does TrakGene offer for managing hereditary diseases?
TrakGene provides advanced digital solutions for genetics professionals, focusing on pedigree chart creation and genomic health record management, which includes a pedigree chart maker that integrates Human Phenotype Ontology (HPO) terms and risk assessment tools.
How do TrakGene’s tools benefit genetic advisors?
The tools streamline data collection and enhance the accuracy of evaluations related to hereditary diseases, leading to more informed healthcare decisions and improved patient care and clinical outcomes.
What security standards does TrakGene adhere to?
TrakGene complies with HIPAA and GDPR standards and implements an ISO27001 Information Security Management System to ensure the security of genetic data.
What causes Sickle Cell Disease (SCD)?
SCD is caused by a mutation in the HBB gene, resulting in abnormal hemoglobin that distorts red blood cells into a sickle shape, leading to blockages in blood vessels and various complications.
What role do genetic counselors play in managing Sickle Cell Disease?
Genetic counselors educate families about inheritance patterns, guide them through SCD management strategies, and assist with family planning and access to early screening initiatives for timely interventions.
What management strategies are recommended for Sickle Cell Disease?
Recommended strategies include regular health check-ups and the implementation of disease-modifying therapies to alleviate complications associated with SCD.
What is the genetic mechanism behind Cystic Fibrosis (CF)?
CF is an autosomal recessive disorder caused by mutations in the CFTR gene, which disrupts salt and water transport across cell membranes, leading to thick mucus accumulation in organs like the lungs and pancreas.
How is Cystic Fibrosis inherited?
Both biological parents must be carriers of the CF gene mutation for a child to inherit CF, resulting in a 25% risk of the condition if both parents carry the mutation.
Why is early diagnosis important for Cystic Fibrosis?
Early diagnosis allows for timely interventions that can significantly enhance health outcomes, as comprehensive screening for CF-causing variants is crucial.
What management strategies are used for Cystic Fibrosis?
Management strategies include enzyme replacement therapy for digestion and pulmonary care to address respiratory issues, which are essential for improving quality of life and longevity for individuals with CF.






